Even if you love the benefits of exercise, it can be challenging to make time to work out. That’s the appeal of high-intensity interval training, known more commonly as HIIT. It promises the best workout in the least amount of time. And evidence suggests it delivers: In as little as seven minutes per session, it can offer many long-term benefits to metabolic health, including better glucose processing and improvements in insulin sensitivity.
But you may also see that HIIT prompts a short-term spike in blood sugar levels or headlines suggesting that intensive training may cause cellular damage. Although neither are things to worry about, it’s worth unpacking the research. Here’s what you need to know about HIIT’s short- and long-term effects on your health.
What Is HIIT?
Definitions of high-intensity interval training vary, but the American College of Sports Medicine defines it as any kind of workout that alternates five-second to eight-minute-long bursts of intense activity, where your heart rate reaches 80 to 95 percent of its maximal capacity (often defined as your age subtracted from 220) with equal or longer periods of partial or complete rest performed at 40 to 50 percent of your max heart rate.
Within those parameters, you can create all kinds of HIIT workouts—whether running, cycling, doing bodyweight exercises at the gym, or some combination of all of the above. When it comes to research-backed iterations, one popular style is Tabata, where you do eight rounds of 20 seconds of intense exercise followed by 10 seconds of rest; another is the 10-by-1 method, which involves 10 one-minute bursts of activity, each followed by one minute of recovery. Or there’s the 4-by-4 method, where you do four four-minute intervals, each followed by a three-minute recovery period. You can even do as little as three rounds of 20-second all-out efforts, each followed by two minutes of recovery, according to one much-publicized 2016 study in the journal PLOS One. (All of these should be preceded by a warmup and followed by a cooldown.)
Those short bursts of work trigger the same metabolic pathways as continuous, moderate-intensity exercise—except they do it much faster because they require more immediate fuel than a less-hardcore sustained effort. That leads to significant health outcomes, like increased calorie burning, fat burning, cardio fitness, and decreased blood pressure.
What Are the Metabolic Health Effects of HIIT?
To understand exercise’s effects on metabolic health, it’s helpful to start with a quick refresher on how energy is produced in the body: Glucose, a simple sugar that comes from carbs, is the body’s most easily accessible source of fuel. Glucose within the bloodstream can be used for immediate energy or stored in the liver and muscles as glycogen. When the glycogen stores are called upon to provide energy, the glycogen is converted back to glucose.
“I don’t think people should worry about the acute increase in blood glucose from exercising. That’s just your body responding to a stressor as it should. That’s what we want our body to do.”—Matthew Laye, PhD
Increased energy expenditure—AKA exercise, especially high-intensity exercise—activates adenosine monophosphate-activated protein kinase (AMPK). This enzyme mobilizes GLUT4 glucose transporters that help your muscles extract glucose from the blood for energy. If there isn’t enough glucose in the blood, your body turns to its glycogen stores. Glycogen in the muscles can only be used by the cells where it is stored, but glycogen stored in the liver can be dispersed throughout the body. As a result, muscle and liver glycogen together become the body’s primary energy source during intense exercise.
As a result of this shift in energy use, it’s normal and healthy for blood sugar to rise during exercise because your muscles and other organs need that extra fuel to meet the physical demands you’re asking of them. HIIT also increases the production of catecholamines, hormones released into the body in response to physical or emotional stress and known to affect your body’s glucose response. That rise in catecholamine levels causes a 7x-8x increase in glucose production, even while glucose use only increases 3x-4x. However, that same review also found in multiple studies that HIIT workouts reduced average glucose for up to three days after the workout in subjects with and without diabetes.
“I don’t think people should worry about the acute increase in blood glucose from exercising,” says physiologist Matthew Laye, PhD, associate professor at the Idaho College of Osteopathic Medicine. “That’s just your body responding to a stressor as it should. That’s what we want our body to do.”
Scientific research further supports HIIT’s benefits: Doing three HIIT workouts a week for up to 12 weeks improved aerobic capacity (a measure of how well the heart and lungs get oxygen to your muscles), blood pressure, and fasting glucose in people who were overweight or obese, according to a 2017 review of 65 studies published in the British Journal of Sports Medicine. When done longer than 12 weeks, HIIT improved even more cardiometabolic risk factors, including waist circumference, body fat percentage, resting heart rate, and systolic blood pressure. Interestingly, these metabolic improvements weren’t seen in normal-weight people, though HIIT still improved their aerobic capacity. The authors say that more research is needed to determine why.
The 2017 review suggests multiple possible mechanisms support the metabolic health benefits of HIIT, including increased production of the fat-burning hormones catecholamines, activation of AMPK to aid glucose clearance from the blood, as well as improved endothelial function, which plays a vital role in the widening of blood vessels, ultimately reducing blood pressure.
Of course, you can’t talk about glucose without mentioning insulin, a hormone made in your pancreas. One of insulin’s primary roles is clearing excess glucose from the blood by shuttling it into cells or directing it into storage. During exercise, when your body needs easy access to glucose, the fuel storage effects of insulin are suppressed, and insulin production is inhibited. But physical activity makes your body more sensitive to the insulin that is available, so your muscle cells are better able to use it to take up glucose during and after working out.
So what happens to your glucose and insulin post-exercise? The more intense your workout, the more fuel you use—and the longer it will take your body to replenish those stores and restore normal blood sugar. And despite the short-term spike it may cause, exercising can take some of the pressure off your pancreas to produce insulin to lower glucose levels.
That’s because exercise activates the GLUT4 glucose transporter mentioned earlier, which docks into cell membranes, allowing glucose to pass into the cell. “That glucose transporter is the same one that’s activated by insulin,” Laye explains, which is why when you exercise after a meal, your body doesn’t need as much insulin to bring your glucose levels back down. This is a key benefit to exercise because high insulin levels are linked to numerous adverse health effects: Too much insulin in your body can lead to insulin resistance, which increases the risk of Type 2 diabetes and plays a role in cardiovascular complications, the development of Alzheimer’s disease and breast or prostate cancers, and several other diseases.
Can Stress from High-Intensity Exercise Be Bad for Health?
One misconception about HIIT is that the stress it puts on the body can have negative repercussions. For example, a recent study published in the journal Cell Metabolism showed that excessive exercise training caused mitochondrial functional impairment and decreased glucose tolerance in healthy volunteers. However, this evidence doesn’t detract from the exercise’s benefits—let’s unpack why.
Exercise is a stressor, and your body responds to it by burning energy for fuel. That happens on a cellular level, where your mitochondria—organelles known as the power plant of cells—convert potential energy from food molecules into ATP, a molecule that is responsible for storing and releasing energy in the body. Glucose is largely dependent on mitochondria to generate energy in cells.
All exercise increases mitochondria. This increases aerobic capacity—AKA how efficiently your body uses oxygen—because the more mitochondria you have, the more aerobic energy you’ll be able to produce. And aerobic energy is fueled by glucose. Typically, you get that mitochondrial benefit in lower-intensity aerobic workouts. But in a 2018 study, a HIIT workout (either five four-minute cycling sessions at 75 percent peak effort, each separated by one minute of rest, or four 30-second sprints at maximum effort, each separated by 4.5 minutes of recovery time) produced a similar response in mitochondrial function as longer moderate-intensity workouts (30 minutes of continuous exercise at 50 percent peak effort).
The Cell Metabolism study mentioned earlier appeared to demonstrate that if exercise gets too excessive, it might decrease mitochondrial function and increase the risk of metabolic dysfunction. But the type of excessive exercise used in that study was more like short-term overtraining, not the kind of workout even the most ardent home athletes would do consistently. Moreover, the detrimental glucose impacts attributed to the exercise were limited, transient, and likely not significant long-term.
Related article:
Outside of that study, “I think HIIT has almost universally been shown to be beneficial for longer-term glycemic control in both healthy and people with metabolic conditions whether it’s cardiovascular disease, Type 2 diabetes, prediabetics, cancer patients,” says Laye.
High-intensity training improved insulin sensitivity for up to three days after exercise in people with and without a metabolic health condition, according to an older meta-analysis published in the journal Diabetes, Metabolic Syndrome and Obesity. That same study showed that high-intensity training improved fasting glucose and insulin sensitivity in as little as two weeks. A more recent study published in the Scandinavian Journal of Medicine & Science in Sports confirmed that HIIT increased glucose metabolism in muscles and insulin sensitivity in people with Type 2 diabetes after just two weeks of HIIT.
What’s the Best Way to Incorporate HIIT into My Routine?
When it comes to HIIT, “it’s not an everyday type thing, and that’s the beauty of it,” says Laye. “You don’t need a lot of it.”
The U.S. Department of Health and Human Services guidelines recommend 75 minutes of vigorous aerobic activity a week. That could break down into two 35- to 40-minute workouts, three 25-minute workouts, or more shorter workouts (even 10-minute exercise sessions count towards your weekly minutes). Depending on your fitness level, you can do up to 150 minutes a week of vigorous-intensity aerobic physical activity.
The guidelines don’t define “vigorous” as HIIT specifically. Still, some experts recommend HIIT training no more than three times a week, as the higher intensity can lead to excess inflammation and may increase injury risk. Indeed, a 2020 study published in Frontiers in Physiology found that intense, extended exercise increased markers of inflammation. The point: Your body needs time to recover between workouts, and that’s where lower-intensity workouts (which have their own benefits!) come in.
Final Thought
Compared to low or moderate-intensity longer-duration training, HIIT promotes superior and faster adaptations in glycemic control and overall metabolic health, and these positive adaptations are even retained over more extended periods.
 Learn how HIIT affects your metabolic health
Learn how HIIT affects your metabolic health
Levels, the health tech company behind this blog, can help you see the impact of factors like diet and exercise on your metabolic health. Get access to the most advanced continuous glucose monitors (CGM), along with an app that offers personalized guidance so you can build healthy, sustainable habits. Click here to learn more about Levels.

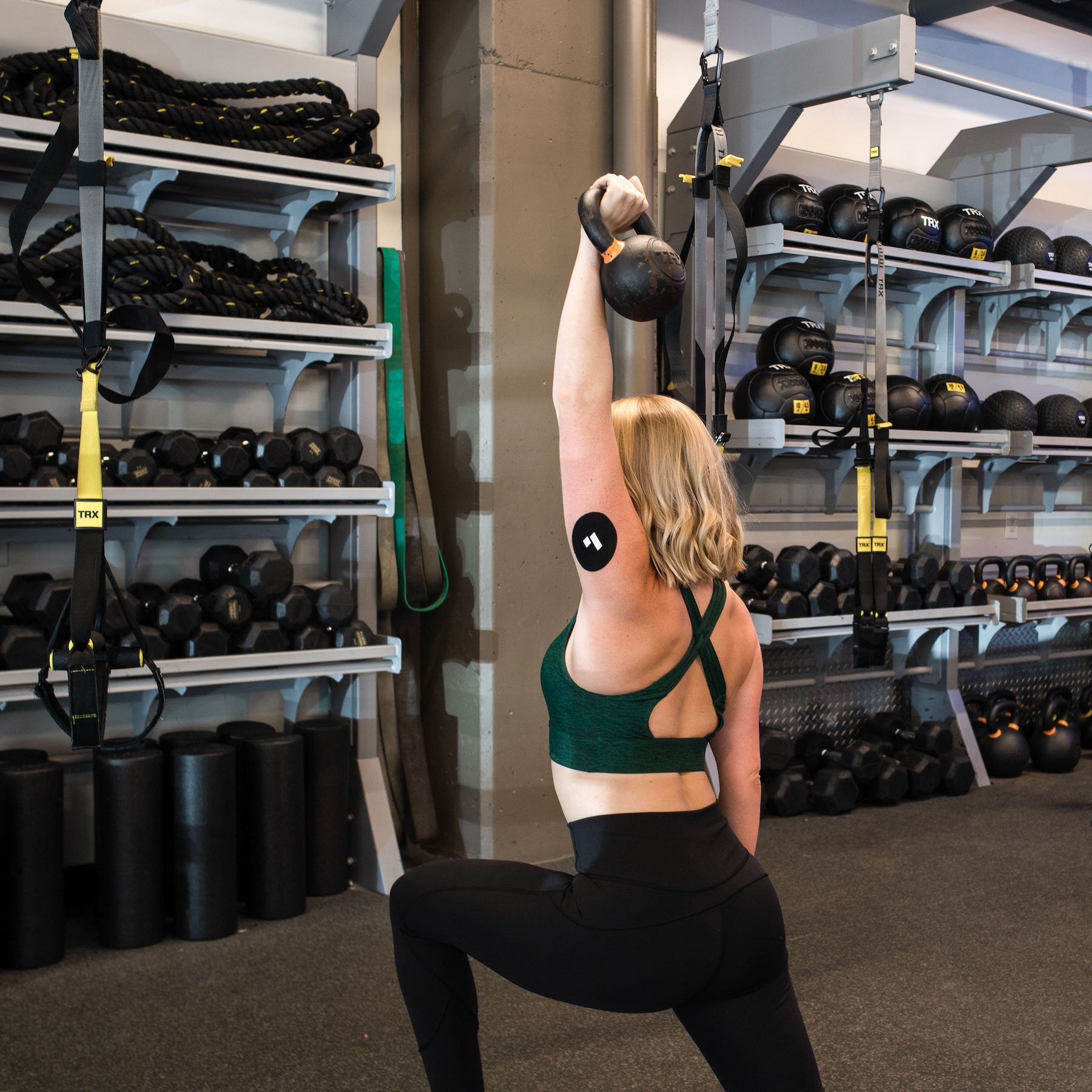
 Learn how HIIT affects your metabolic health
Learn how HIIT affects your metabolic health






