Rates of good metabolic health in American adults are concerningly low. Currently, only 12% of Americans meet the criteria for metabolic health. Even people within normal weight range aren’t necessarily metabolically healthy and may still show elevated glucose and cholesterol levels.
Not coincidentally, average sleep duration has decreased from 9 hours per night 100 years ago to 6.8 hours per night today.
Getting consistent, quality, and uninterrupted sleep is a critical component of preventing chronic diseases such as Type 2 diabetes, obesity, heart disease, Alzheimer’s disease, and stroke–all of which are linked to metabolic dysfunction. Unfortunately, these prevalent conditions are rising, affecting hundreds of millions of Americans.
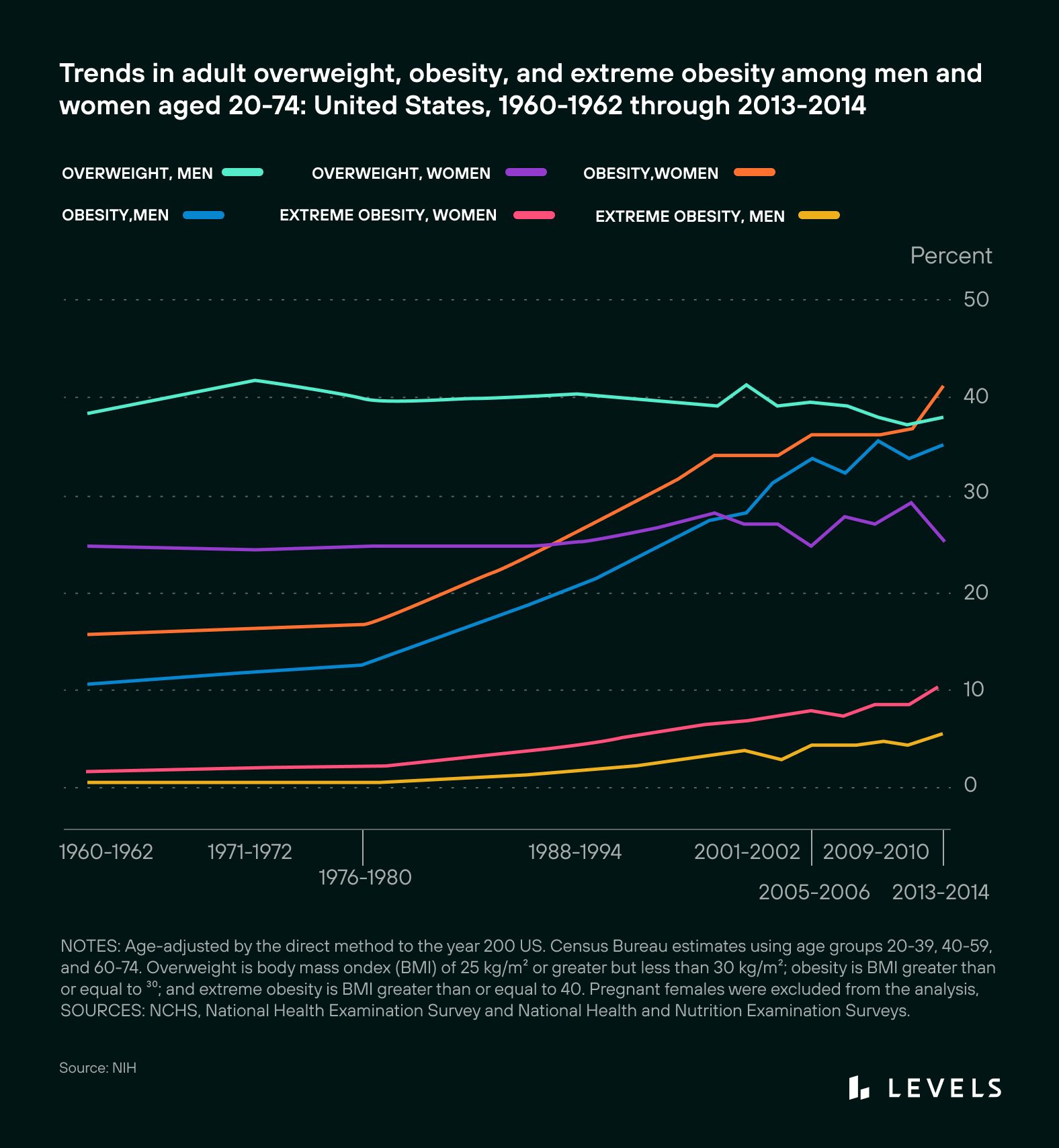
Increasing rates of obesity over time. Source: NIH
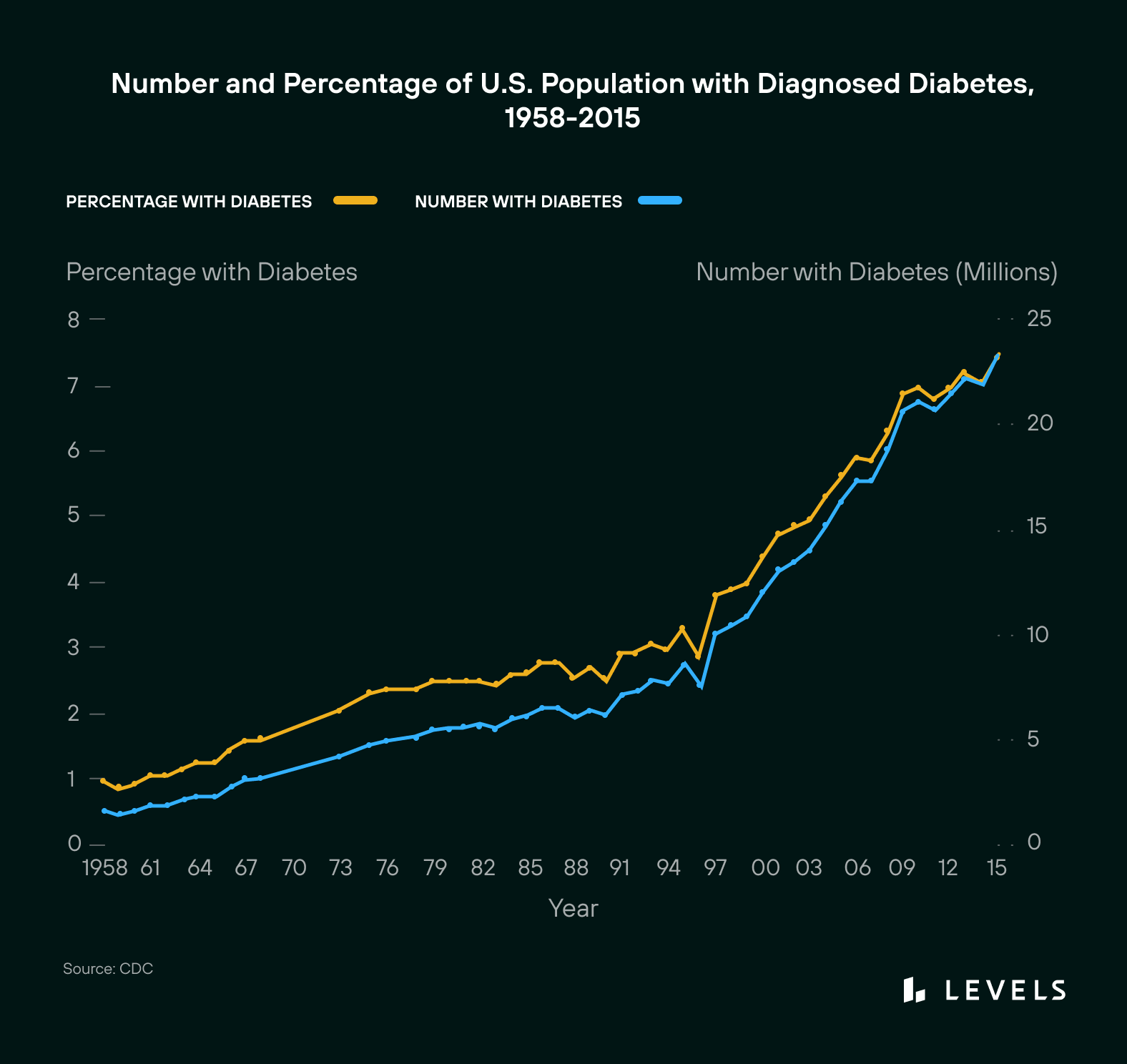
Increasing rates of diabetes over time. Source: CDC
What is Metabolic Health?
Your metabolism is a fundamental component of overall health. It’s your body’s ability to process, utilize, and store energy from food.
We can understand our metabolic health by examining our blood sugar levels, insulin, cholesterol, blood pressure, and weight.
Since metabolism is core to our overall health, metabolic dysfunction can wreak havoc on multiple fronts. If our metabolic metrics are out of whack, we can suffer from a myriad of unpleasantries such as weight gain, anxiety, balding, dementia and memory impairment, depression, and more. Further, chronically elevated glucose levels are linked to diabetes, a condition characterized by metabolic dysfunction.
To further complicate one’s understanding of their metabolism, everybody is unique and responds to factors differently. For example, the same banana could spike Person A’s glucose levels and have minimal effect on Person B. This is why any standardized “perfect” diet is theoretically impossible.
Insulin is vital: Your body releases it when glucose enters the bloodstream to help cells absorb it.
“The magic number for metabolically-optimized sleep appears to be between seven to eight hours per night. Less than seven, the risk of diabetes increases sharply for every hour lost. Above eight hours, the risk also increases.”
When our glucose and insulin levels are chronically high, we can develop “insulin resistance,” which means our cells become “numb” to insulin signaling. Ultimately, we would need more insulin to get sugar in the cells. The more insulin resistance we develop, the harder it is for our body to funnel and convert glucose into energy, and we end up with a lot of excess glucose in our bloodstream and converted to fat.
However, the bright side is that since our metabolism is so foundational, pursuing metabolic fitness can theoretically help put us in an advantageous position in a highly multifaceted biological playing field. Modern technology like continuous glucose monitoring (CGM) lets us peek under the hood to see how our body reacts to food decisions in real time.
Metabolic health is also impacted by multiple variables outside of nutrition, such as exercise, stress, and sleep.
Sleep, in particular, can profoundly affect your body’s metabolic health.
How Much Sleep Should I Get to Be Metabolically Healthy?
Even intermittent sleep deprivation can have detrimental effects on our metabolic health.
For example, one study followed 11 healthy young men subjected to six nights of sleep deprivation with four hours of sleep, followed by a week of twelve hours per night. On the fifth day of each scenario, the participants did an intravenous glucose test (a diagnostic test often used to diagnose diabetes) to see how their metabolism reacted to a fixed amount of oral sugar.
The results? The participants exhibited signs of impaired metabolism and insulin resistance during the sleep deprivation period. The rate of clearing sugar out of the bloodstream was 40% slower than when they were well-rested.
This relatively short six-night sleep deprivation period generated metabolic profiles in the otherwise healthy young men that resembled people with Type 2 diabetes.
Another study followed healthy, normal-weight people who fell into the categories of short sleepers (those who slept less than 6.5 hours per night) and normal sleepers (7.5 to 8.5 hours of sleep per night).
The short sleepers had to secrete 50% more insulin than normal sleepers to achieve similar glucose results, placing them at risk of developing insulin resistance in the long term.
Insulin resistance, which acts as a brake on our body’s ability to burn fat for energy, also contributes to weight gain.
In pursuit of metabolic fitness, we want our insulin levels to be relatively low and stable. Sleep deprivation makes this very difficult.
Even a few days of inadequate sleep can negatively impact our metabolic health. However, excessive sleep isn’t necessarily always better for metabolic health.
The magic number for metabolically-optimized sleep appears to be seven to eight hours per night. Any less than seven, the risk of diabetes increases sharply for every hour lost. Above eight hours, the risk also increases.
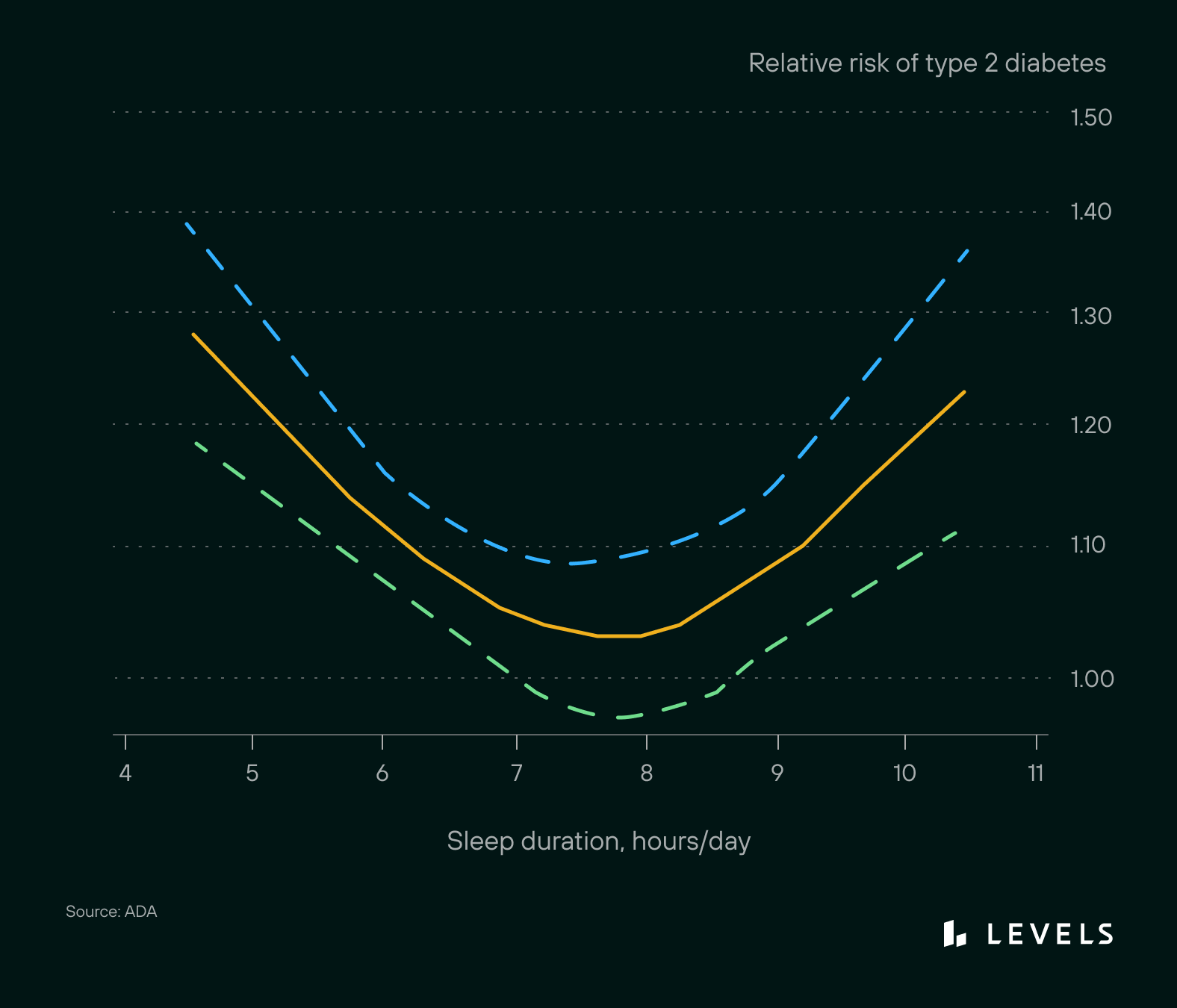
The risk of type 2 diabetes increases with too much or too little sleep. Source: ADA
How Sleep Quality Impacts Your Metabolic Health
Sleep duration is only part of optimal sleep hygiene.
Sleep quality also has a significant impact on metabolic health. One study followed adult men for eight years and found that subjects who reported interrupted sleep and difficulty maintaining sleep had double to triple the risk of developing Type 2 diabetes.
The regulation of glucose and insulin is partially controlled by cortisol (often pegged as our “stress hormone”), which tells our body that something “stressful” is happening and preparing to have the energy to utilize against this real or perceived threat.
To help the body prepare, cortisol mobilizes the stored glucose from the liver into the bloodstream. It also decreases insulin production in the pancreas and reduces insulin sensitivity in the body, which means that the glucose is less likely to be utilized by cells and more likely to remain in circulation, elevating blood glucose levels.
Since our cortisol levels tend to be lower during the evening and early part of the night, our glucose levels tend to stabilize around a lower range at night. Sleep deprivation for just six days can increase cortisol levels, which in turn can elevate blood sugar.
Sleep deprivation can also trigger increased growth hormone, which decreases glucose uptake by the muscles, further contributing to a rise in blood glucose levels.
A lack of high-quality sleep may also increase your appetite, leading to a higher likelihood of overeating.
One study of twelve healthy young men with two days of restricted sleep reported an increase in hunger and appetite for calorie-dense high-carbohydrate foods, an elevation of the hunger hormone ghrelin, and a decrease in the satiety hormone leptin.
Sleep deprivation and inflammation in the body are also tightly linked. Some experiments highlight an increase in pro-inflammatory chemicals like TNF-a, IL-6, and CRP, which are immune markers also increased in Type 2 diabetes and obesity.
Final Thoughts
There are many shared underlying mechanisms between sleep loss and metabolic dysfunction, so it begs the question: how do we improve our sleep?
Optimizing our metabolic health by getting better sleep can start with making small changes: ensuring your bedroom is dark and quiet, ensuring any possible distractions are far away, and limiting your caffeine intake near bedtime.
Erratic sleep patterns often turn our focus to our daily schedules. Carving out an adequate amount of time for seven to eight hours of high-quality sleep can be tricky for the busy, but the research suggests it’s worth our effort.
However, to truly understand how our sleep efforts positively impact our metabolic health, we can leverage objective and personal continuous glucose data to discern the relationship in real time.
Beyond potentially preventing chronic diseases, stable and healthy glucose and insulin levels can positively impact many aspects of our wellness, such as inflammation, memory, immune function, energy levels, skin health, sexual health, and more.








