Introduction
Research shows that persistently elevated glucose levels can accelerate skin aging and create conditions that lead to acne. Monitoring glucose levels with a metabolic tracking tool like Levels can provide actionable insights grounded in personal data that may lead to clearer, more youthful-looking skin.
Aging & Wrinkles
Skin aging, wrinkling, and discoloration are due to various dysfunctions in cellular processes. These include thinner layers of skin, diminished numbers and function of structural proteins like collagen and elastin, reduced blood flow, decreased pigment production, and less cell turnover and replication.
Excess sugar in the body appears to speed up skin aging. This is due in part to “glycation,” the process by which a glucose molecule bonds with proteins, fats, or DNA in a cell, forming what are called “Advanced Glycation End products” (aptly abbreviated “AGEs”) with altered ability to perform normal functions. (You can also get AGEs from external sources, including grilled, fried, or baked foods, and from air pollution.
Glycation can affect tissues all over the body and is implicated in diseases including diabetes, cardiovascular disease, and Alzheimer’s. Still, the skin is particularly susceptible because of how collagen interacts with sugar. Collagen is the most plentiful protein in the human body and is vital to your skin’s structure and resilience.
Glycation alters normal collagen function by causing protein cross-linking, which results in skin stiffness. It also changes the molecular charge of collagen, which prevents the protein from interacting normally with cells and proteins around it. Lastly, glycated collagen resists breaking down, impairing the normal turnover process. This glycation can have long-term consequences. Because collagen has a very slow turnover rate (on the order of decades), once it becomes glycated and dysfunctional, the consequences can last for years.
Glycation can affect other proteins in the skin, including vimentin and cytokeratin. These proteins are also critical for the structural support of skin cells, but glycation reduces the cells’ ability to contract, preventing the skin from moving properly.
The good news is that there are multiple ways to reduce glycation in the body, including diet and lifestyle changes that support metabolic fitness. In fact, studies have shown that tight glycemic control over just four months can reduce glycated collagen by 25%.
Acne
The relationship between glucose, insulin, and acne is well-established, and elevated glucose and insulin are implicated in acne development.
Insulin and insulin-like growth factor 1 (IGF-1) can contribute to acne development. These hormones stimulate oil production in the hair follicle and increase the production and activity of androgens, or hormones like testosterone.
“The skin is the largest organ in the body, and our skin’s health is a clue to our overall well-being.”
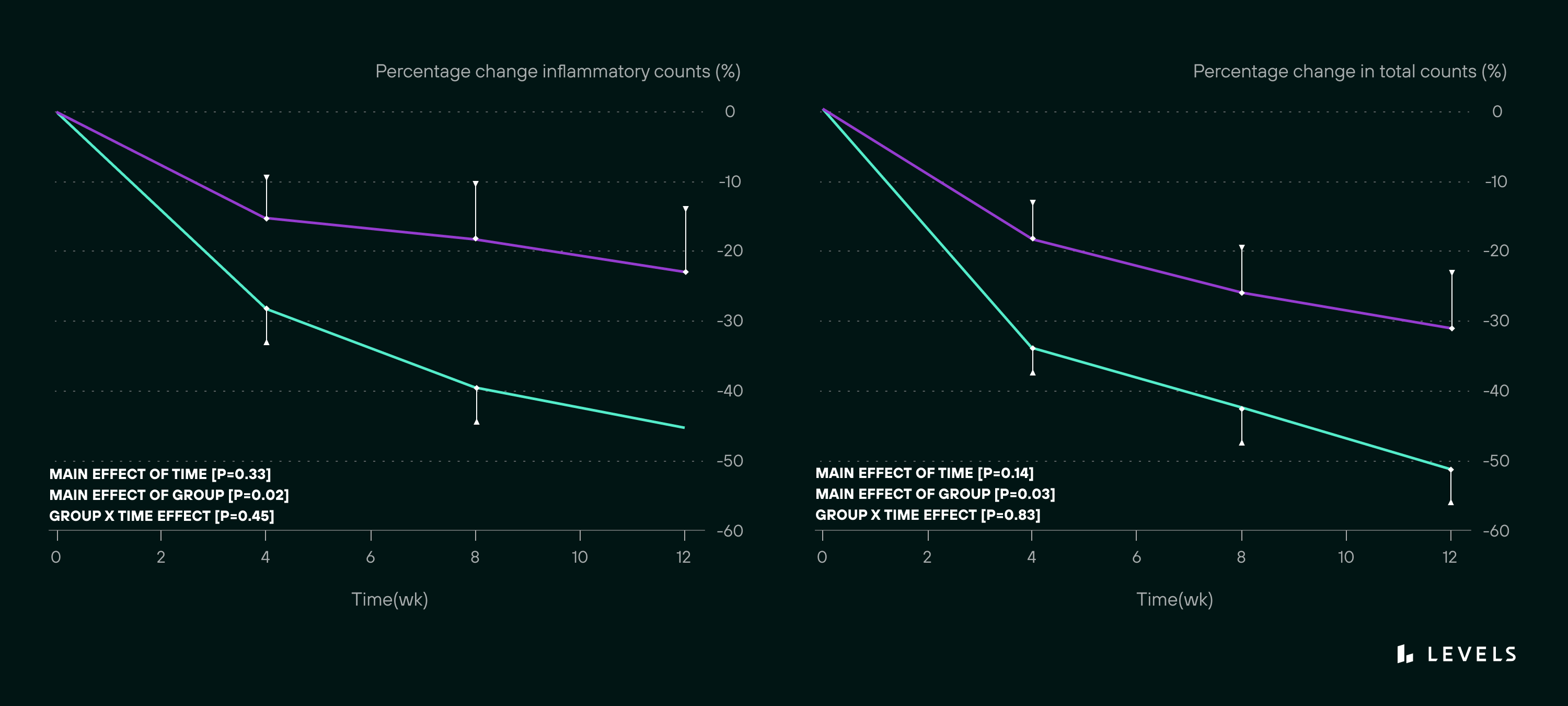
Multiple studies have shown that raised blood sugar also leads to increased acne. A 2007 study followed two groups of male patients aged 15-25 over 12 weeks; the first group consumed a low-glycemic-load diet, meaning diets with less propensity to spike blood sugar. The other group’s diet emphasized carbohydrate-dense foods without reference to glycemic index.
The low-glycemic-load diet not only showed a significantly greater reduction in acne lesions (see Figure 1) but also a reduction in weight and improvements in insulin sensitivity (the ability of the body’s cells to efficiently use available insulin) when compared with the group following the carbohydrate-dense diet.
A 2012 study took this research further by putting participants on a low-glycemic-load diet for 10 weeks while also taking skin biopsies. The study also included a control group instructed to eat high-carbohydrate foods daily. Looking at each group’s skin under the microscope before and after the intervention showed significant differences.
At 10 weeks, the low-glycemic group had significantly fewer non-inflammatory and inflammatory acne lesions and smaller sebaceous (oil-producing) glands. There was also less evidence of SREBP-1, a protein that activates oil production in the skin, and IL-8, an inflammatory molecule—both strongly associated with acne.
Interestingly, those who followed low-glycemic dietary recommendations saw significant acne improvements, even without limiting other foods known to contribute to acne, including dairy.
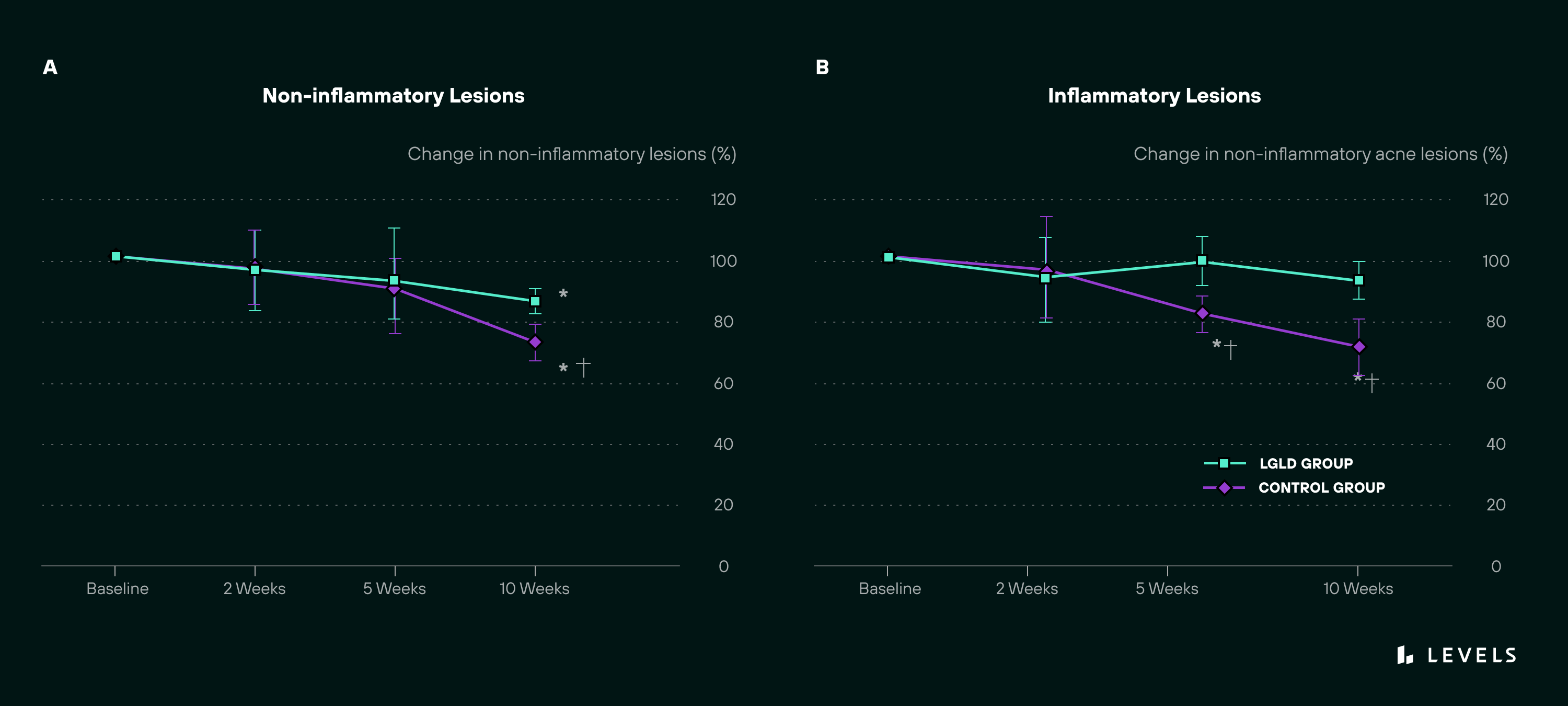
Figure 2: Decrease in acne lesions after 10-week low glycemic diet. Source
Diets with a high glycemic impact also lead to overactivation of the mTOR genetic signaling pathway, leading to increased oil production and cell proliferation, both of which contribute to acne. The genetic pathways that link glucose and acne are still being uncovered, but they contribute even more insight into how dietary choices can benefit skin health.
More recently, a 2023 study found that consumption of sweets correlates with acne severity in young adult women, while a 2020 review found that people who eat lower glycemic load diets have less acne than those who eat high glycemic foods.
Conclusion
The skin is the largest organ in the body, and our skin’s health is a clue to our overall well-being. Reducing premature wrinkles and acne is a concern for many, and it’s essential to consider the underlying biology when approaching how to prevent and treat these conditions. When we better understand the underlying mechanisms that link glucose, acne, and wrinkles, we have even more reasons to strive for dietary choices that optimize our glucose levels, minimize glucose spikes, and improve metabolic fitness.
Research has shown, however, that two people may respond entirely differently to the same food in terms of how much their glucose rises, so how do we know what to eat to optimize our glucose levels? Fortunately, continuous glucose monitoring allows us to track our glucose response to various foods and lifestyle decisions and enables us to adhere to a truly personalized “low-glycemic” diet. The metabolic awareness we develop by monitoring our own biological information in real time can optimize many aspects of our health, including our skin.








