Metabolism is the set of cellular mechanisms that generate energy from our food and environment to power every single cell in the body. When these energy-producing pathways run smoothly, we have optimal metabolic health.
Since all cells in the body require energy to function, metabolic health is foundational for overall health and well-being.
Why would someone want to improve their metabolic health?
- Stable and sustained energy throughout the day
- Sharp memory and recall
- Sustained exercise endurance
- Fat-burning ability and healthy weight
- Stable mood, decreased anxiety and depression
- Clear skin and reduced wrinkles
- Improved fertility
- Improved sexual health
- A high-functioning immune system
- Lower risk of chronic diseases like diabetes, Alzheimer’s disease, obesity, fatty liver disease, heart disease, stroke, and more
What is Metabolic Health?
Clinically speaking, metabolic health is defined by optimal levels of five markers: blood sugar levels, triglycerides, high-density lipoprotein (HDL) cholesterol, blood pressure, and waist circumference—without using medication. We can improve most of these markers by consistently making choices that keep glucose levels stable and healthy.
The opposite state is known as metabolic syndrome, where people have three or more of the following traits:
- A waistline of 35 inches for women and 40 inches for men
- Fasting glucose above 100 mg/dL
- HDL cholesterol less than 40 mg/dL
- Triglycerides above 150 mg/dL
- High blood pressure (130/85 or higher)
Can You Improve Your Metabolic Health?
We often talk about metabolic fitness because fitness is not an inherent characteristic or something that “happens to us.” Instead, fitness is something that can improve when we put in consistent work and training. And just like physical fitness, metabolic fitness improves when we put in the effort and make the necessary lifestyle changes.
Let’s take the analogy of starting a running program to improve our physical fitness to run a marathon. Our first jog isn’t going to be 26.2 miles; it’s likely going to be a short slog. But, as we lace up our shoes each day, hit the pavement, and track our progress over time, we see and feel progress. We notice minor adaptations in our bodies signifying improved cardiometabolic health: our breathing might get easier as we sprint up hills, our body composition becomes more defined, and maybe our mood improves. We might track our mileage in Strava or our heart rate with a Fitbit and get excited as these metrics start to improve. As the weeks of running progress, it is clear that our physical fitness is improving.
On the flip side, if we decide to take a few months off from training, physical fitness will likely decline: those hard-earned gains in muscle mass may diminish, and we’d likely feel more winded the first time we get back out there.
Learning how to improve metabolic health is no different. If we make daily choices that support metabolic processes, we will adapt to develop better metabolic fitness. We might not see our muscles grow, but inside our bodies, the microscopic machinery involved in converting fat and glucose to energy becomes more efficient, and our resting metabolic rate improves. While becoming physically fit requires regular exercise (a combination of resistance training, interval training, and more endurance-based cardiovascular training is ideal), becoming metabolically fit involves consistent smart decisions about diet (including what to eat, when to eat, and how to pair foods), sleep, stress management, physical activity, and exposure to metabolism-disrupting environmental toxins. Our current level of metabolic fitness is highly dynamic and mainly in our control.
Just like we can track metrics of physical fitness to keep us informed, on track, and motivated, we can also now track our metabolic fitness. Since glucose is the primary energy-building block for our metabolism, tracking this biomarker can give us helpful insight into our level of metabolic fitness.
And, just like with physical fitness, we can see meaningful improvements in our lives even if we haven’t won an Olympic gold medal. Fitness is a spectrum, and each small amount of improvement is a win. As with most processes in the body, there is not an “on-off” switch for metabolic health. We are not either “healthy” or “unhealthy.” Instead, we are on a metabolic continuum, and our choices—coupled with our genes—determine where we stand each day.
 Want to learn more about your metabolic health?
Want to learn more about your metabolic health?
Levels, the health tech company behind this blog, can help you improve your metabolic health by showing how food and lifestyle impact your blood sugar. Get access to the most advanced continuous glucose monitors (CGM), along with an app that offers personalized guidance to build healthy, sustainable habits. Click here to learn more about Levels.
How Does Glucose Relate to Metabolic Health?
Glucose is a simple sugar that is a breakdown product of the carbohydrates that we eat. When glucose enters the bloodstream, it signals to the pancreas to release insulin, a hormone that tells cells to absorb glucose. The mitochondria process some of this glucose to form energy (called ATP) that our cells can use. Excess glucose is stored in the muscle and liver as glycogen and can also be converted to triglycerides and stored in fat cells.
When the body needs energy, it can tap into glucose from the bloodstream, stored glycogen in the muscles or liver, or even make new glucose from other compounds like amino acids (breakdown products of proteins). Aside from using glucose for producing energy, our bodies can also break down stored fat to make energy and convert protein breakdown products to energy.
However, when our bodies are taxed with processing too much dietary glucose over long periods, it throws off the balance of these processes and leads to health problems. First, chronic excess glucose causes the repeated release of insulin. Over time, high insulin levels can cause cells to become “numb” to insulin’s effect, a process called insulin resistance, the opposite of insulin sensitivity. When this happens, less glucose can enter the cells, so circulating glucose rises. Second, high insulin levels block stored fat from being broken down and used for energy. So, ironically, too much energy in the form of glucose leads us to have more trouble using energy effectively.
Aside from these issues, excess glucose in the bloodstream causes inflammation (immune activation), oxidative stress (an overabundance of damaging free radicals in the body), and glycation (glucose getting “stuck” to things in the body and causing dysfunction).
Given how many deleterious side effects excess glucose can have, it is not surprising that the majority of common chronic diseases are rooted in poor glucose control, including Type 2 diabetes, obesity, heart disease, stroke, dementia, infertility, and more. This is a relatively modern phenomenon: we used to die of infectious disease and starvation. Now, we die of metabolic disease, the modern public health crisis.
Why might that be? For starters, we (on average) eat nearly 10x more sugar per day than we did 100 years ago. Many of us don’t even realize it because sugar is so ubiquitous in our food culture, and it wears many masks (link: 56 names for sugar). Imagine a factory getting 10x more shipments of raw material and trying to just “make it work.” It wouldn’t. The factory would fall apart. The machines would break. The workers would resist to protect themselves. This is what is happening to our bodies. Additionally, too much dietary fat can impair glucose processing; in fact, excess saturated fat impairs the function of the insulin receptor, leading to more circulating glucose.
In short, excess energetic precursors like glucose and fat gum up our bodies’ machinery and are at the root of a vast amount of disease and suffering globally.
“Our lifestyles today are unrecognizable compared to prior centuries.”
Currently, only 12% of Americans have good metabolic health. The other 88% display one or more features that indicate that they have metabolic dysfunction and that their bodies can’t utilize and process fat and carbs efficiently. In this research study, to be considered “metabolically healthy,” you had to have normal blood glucose, triglycerides (a form of fat generated from excess glucose), high-density lipoprotein cholesterol, blood pressure, and waist circumference without needing medications.
Learn more:
What are the Consequences of Poor Metabolic Health?
What do metabolic dysfunction and poor metabolic health and fitness look like? It can be both overt and subtle.
Moreover, metabolic dysfunction looks like weight gain and obesity (dysfunctional body fat storage, often measured by body mass index), insulin resistance and diabetes (dysfunctional glucose processing), non-alcoholic fatty liver disease (dysfunctional management of glucose and fat in the liver), cancer (cancer cells thrive on excess sugar), Alzheimer’s disease (now being called type 3 diabetes, with evidence of insulin resistance in the brain), cardiovascular diseases like heart attack and stroke (damage to vessels from inflammation and excess glucose), and chronic kidney disease (vessels of the kidney impaired by excess glucose).
But more subtly, poor metabolic health can look like the full spectrum of daily pain points of modern living that keep us from reaching our full potential and goals: fatigue, brain fog, depression, anxiety, lack of exercise endurance, infertility, balding, erectile dysfunction, acne, chronic pain, increased appetite, and more.
The key is this: since every cell type needs energy to function, metabolic dysfunction doesn’t discriminate. When our metabolic health is not optimal, the effects can be vast and diverse, subtle and overt.
What are the Risk Factors for Poor Metabolic Health?
Previously, we mentioned that current research shows that 88% of Americans are not metabolically healthy. What’s more, 71.6% of the US are overweight or obese, 120 million Americans are living with diabetes and prediabetes, and 25-40% of the US suffers from largely preventable non-alcoholic fatty liver disease (NAFLD). Why are we seeing such high prevalence of poor metabolic health and its downstream consequences? Our genetic code has not appreciably changed in the time that these diseases have become epidemic, but our lifestyles are unrecognizable as compared to prior centuries.
Some of the risk factors for our poor metabolic fitness (all of which are modifiable in our individual lives):
- Chronic “overnutrition”: We are exposed to a vastly increased amount of food than ever before in history, and our cellular factories haven’t evolved to cope with this level of incoming energy. We eat nearly 10x more sugar per day than 100 years ago. This stimulates the pancreas repeatedly to make insulin (the hormone that helps cells take up glucose), and the cells eventually become numb to this hormone. The liver becomes dysfunctional as excess glucose is converted to fat and stored in it, and the muscles become insulin-resistant and unable to use glucose effectively. Even “normal weight” people can have this kind of dysfunction.
- We are more sedentary than ever.
- Chronic sleep deprivation appears to be the norm, significantly affecting our energy-processing ability.
- Our environmental and synthetic toxin exposure impairs the mitochondria and metabolism.
- Most energy intake among people in the US comes from ultra-processed foods and beverages.
- The experience of psychological stress appears to be increasing, creating elevated cortisol and a hormonal cascade that promotes energy storage rather than use.
- Eating late at night and snacking frequently — common practices in modern life — can result in higher levels of insulin that block fat usage for energy in the body.
How does Blood Sugar Reflect Metabolic Health?
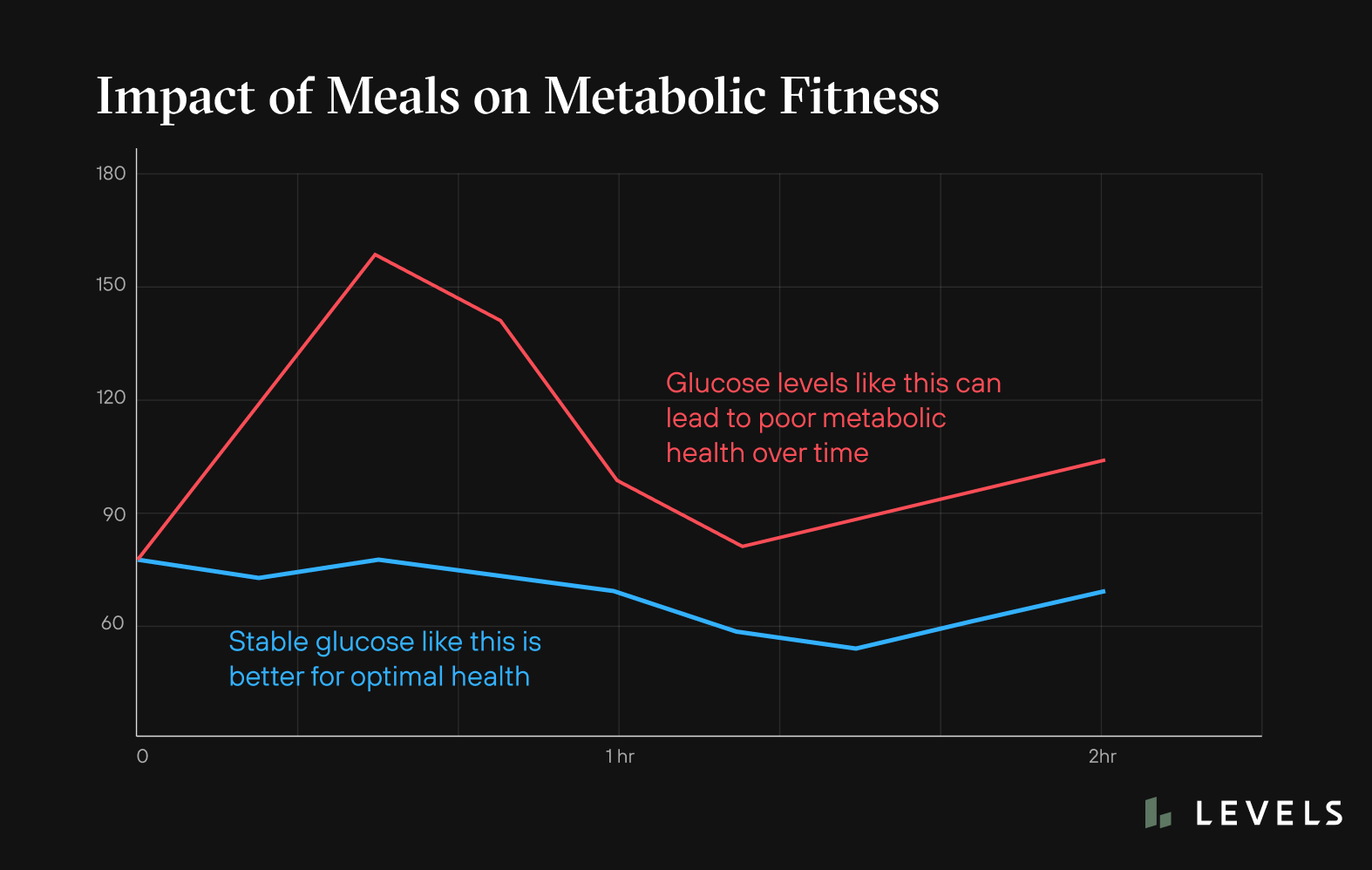
If your metabolic machinery is working optimally, your blood sugar responses will look like:
- Minimal rise of glucose after meals
- A quick return of glucose to baseline after meals
- Maintaining 24-hour glucose levels in a fairly narrow and healthy range
- Keeping fasting glucose (glucose levels measured after consuming no calories for at least 8 hours) in a healthy, low-risk range
Learn more:
Poor metabolic health looks more erratic, spiky, and elevated. Some of this might relate to our body’s response to insulin, knowing that excessive exposure to glucose and fats can promote insulin resistance. When our cells become insulin resistant, they have more difficulty taking up glucose, so we may see:
- Higher glucose peaks after meals
- More extended time periods of elevated glucose after meals
- Morning glucose levels higher than desired
- “Basal” glucose (the glucose level in between meals) is high
- More up-and-down glucose variability during the day
Paying attention to how your blood sugar responds to your diet and lifestyle is a significant first step in improving metabolic health. A continuous glucose monitor is one of the best tools for this job, but you can also do it with a glucometer. Given that diverse and contradictory health and dietary messages come at us from all angles, it can be helpful to have an objective data stream that tells us continuously whether we are staying on track in keeping glucose stable.
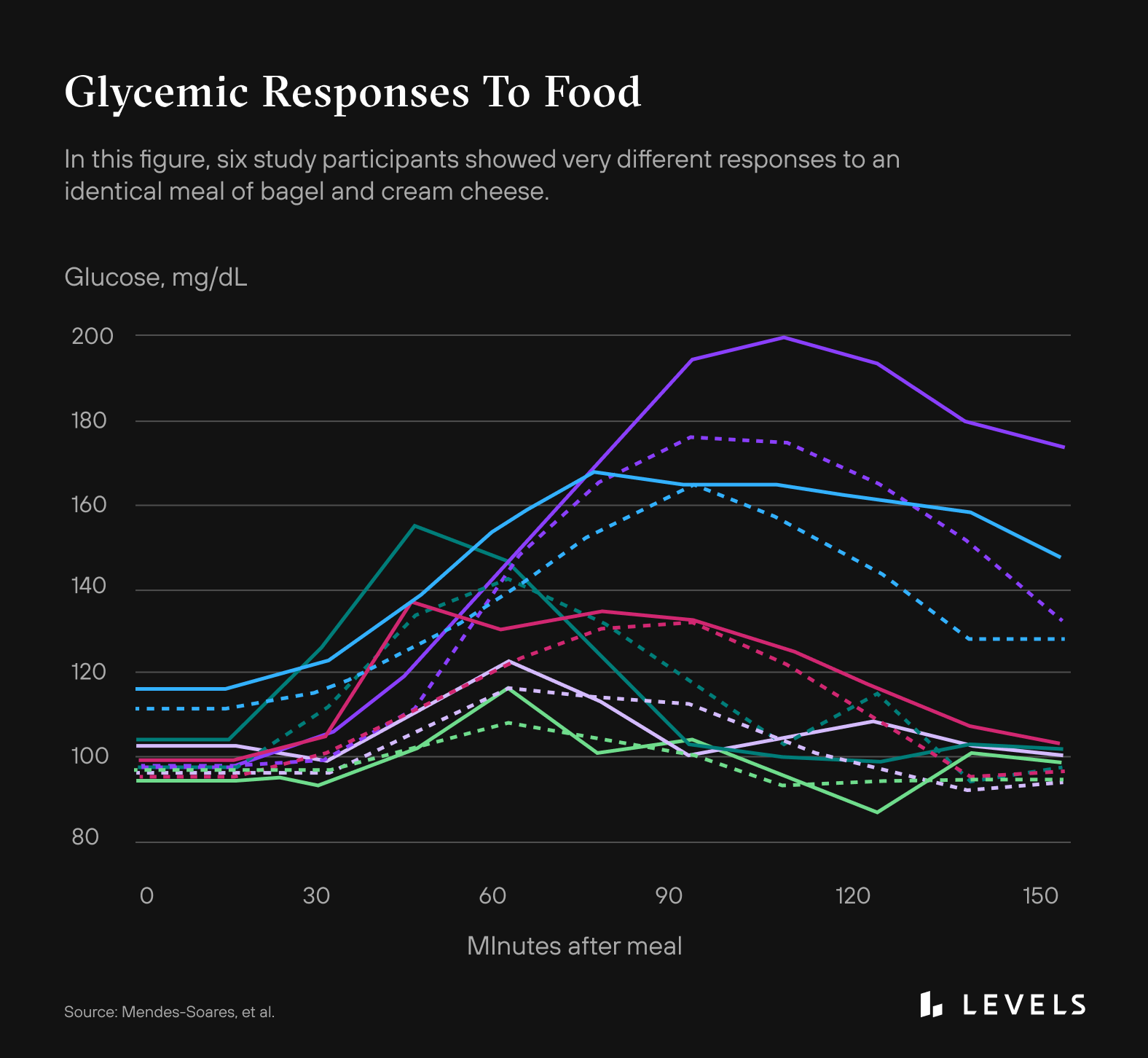
By tracking glucose, we can identify how food and lifestyle choices directly impact our metabolic health with a closed feedback loop that fosters rapid learning and the ability to modulate. People can have very different glucose responses to the exact same food, so knowing how you are personally affected by a particular meal is critical.
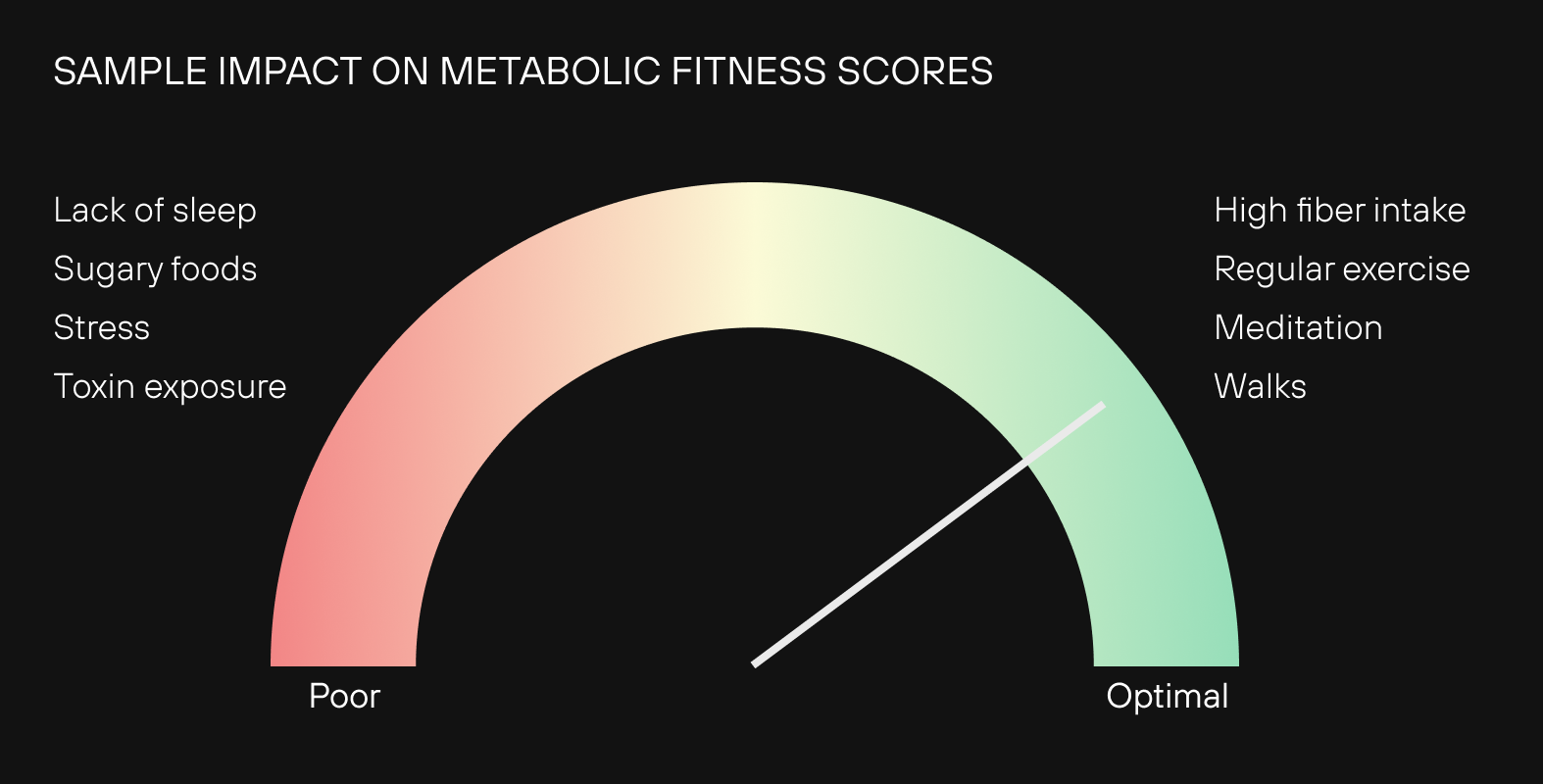
Many strategies for improving metabolic health include eating less refined foods (which make up a significant number of calories among Americans), pairing carbohydrates with protein to exercise, prioritizing sufficient protein intake, and engaging in a mindfulness practice. Behaviors like walking after meals, eating fiber, and regular exercise (building muscle is especially important) will likely contribute to better scores, plus numerous health benefits in general. If you didn’t sleep well or ate foods that spike your blood sugar, you may find your metabolic fitness score lower, between 40 and 60. The average Levels user has a metabolic fitness score between 70 and 80.
Three Key Takeaways
Metabolic health takes practice.
Developing metabolic fitness and maintaining good metabolic health requires effort and repetition. Just like the process of improvement in athletics, martial arts, meditation, or any other practice, consistency is vital.
We can all improve.
Some of us are closer to our metabolic health goals than others, but no one is perfectly metabolically fit. The body is a dynamic machine, and metabolic optimization is a daily, continual process.
You are in control.
Your metabolic fitness level is not a predetermined trait, it’s a description of your current state: constantly in flux and always adaptable. You can make simple, informed decisions each day that can improve the metrics that define your metabolic health.

 Want to learn more about your metabolic health?
Want to learn more about your metabolic health?