Sharp drops and spikes in glucose are often a point of interest for many people exploring their metabolic health.
The reason your glucose level is dropping while sleeping could be due to a wide variety of issues described below.
The Impact of REM Sleep on Glucose Levels
Research also shows that glucose levels decrease by an average of 5% during REM sleep compared to non-REM sleep stages, which may contribute to periodic dips seen at night in nondiabetic people. In fact, healthy people who have glucose dips below 70 mg/dl have twice as many dips at night compared to the day.
Meal and Alcohol Timing and Glucose Levels
When you wake up after a long night’s sleep, your body has been in a fasting state for quite a few hours. During this fasting period, your body expends circulating and stored glucose to perform all the usual physiologic processes. If you tend to stop eating earlier in the evening and do not snack at night, this fasting window will be greater, leading to lower glucose levels during that night.
Additionally, drinking alcohol in the evening could lead to low glucose values overnight. It’s thought that drinking alcohol decreases the liver’s ability to make new glucose via gluconeogenesis, leading to lower circulating glucose levels. To counter this decrease, alcohol stimulates the breakdown and release of stored glucose (glycogen). This balance between impaired gluconeogenesis (new glucose product) and increased glycogenolysis (stored glucose release) means that alcohol shouldn’t significantly affect glucose levels for normal, healthy individuals eating a standard diet.
However, the situation is different for those who’ve been fasting or are in a ketogenic state because these individuals already have much less glucose stored as glycogen in the liver and muscles. Normally this state prompts the liver to produce new glucose via gluconeogenesis, but, as noted above, alcohol inhibits this process. The result is that glucose levels can fall to dangerously low levels, and in extreme cases, this hypoglycemic state can lead to seizures, coma, or death.
Pressure-Induced Sensor Error
Your glucose levels might not actually be dropping at night; it could just be your sleeping position, causing a Continuous Glucose Monitor (CMG) sensor error.
One study found that individual sensors intermittently exhibited unusual glucose readings greater than 25 mg/dl away from the subject’s median of 70-110 mg/dl during sleep. These odd dips were strongly correlated to subjects lying on the sensors.
The analysis also stipulates that the cause of the dip could be due to local blood-flow decreases caused by the compression of tissue in the sleeping position.
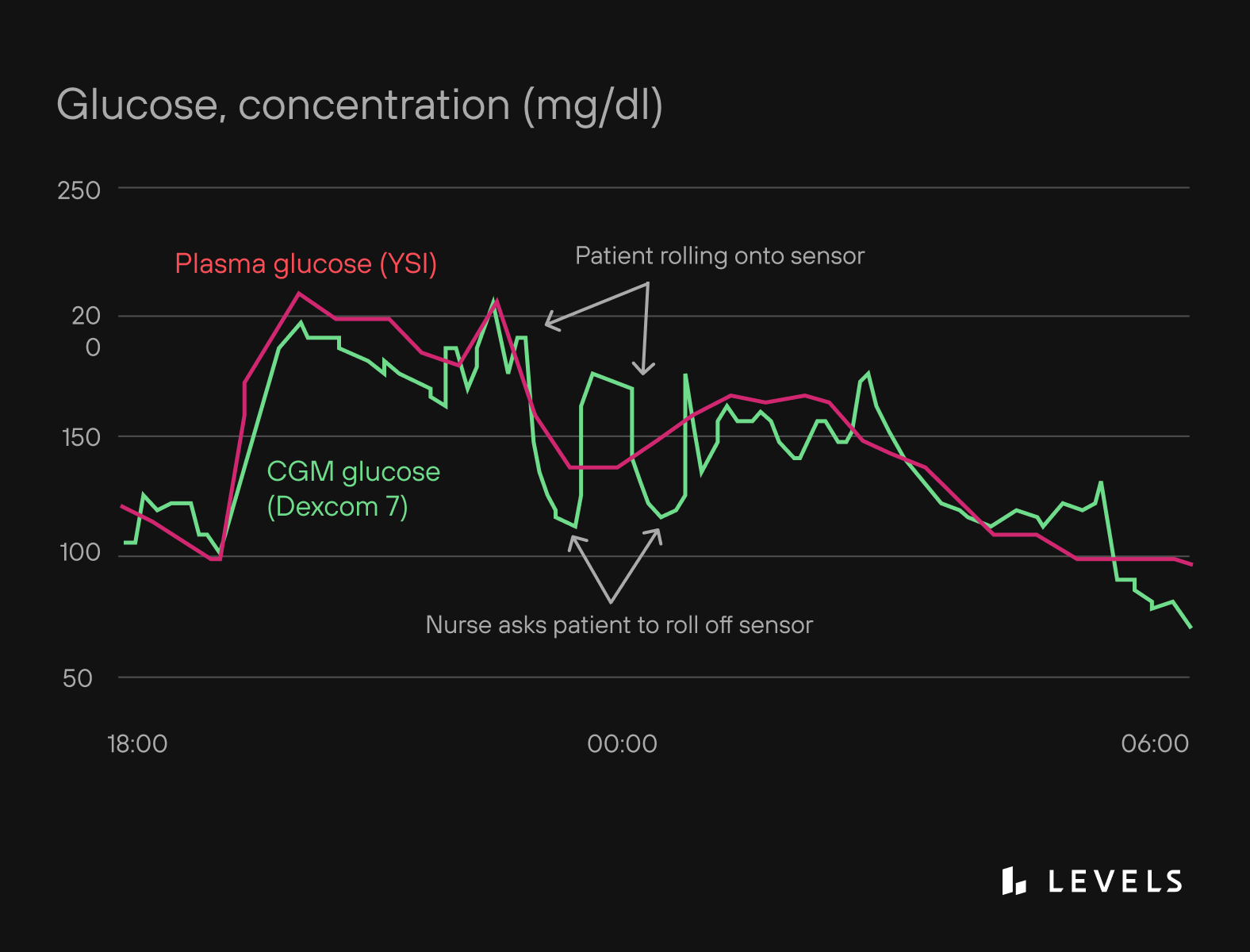
Source: Helton, et al.
Another study confirmed the claims that some glucose dips could be the effect of motion and pressure on glucose sensors. If you lay on the sensor, you could see a dip in the readings that isn’t actually expressive of your real blood glucose content.
To get more accurate readings at night, you can try to adjust your sleeping position in a way that doesn’t put a lot of pressure on the sensor.
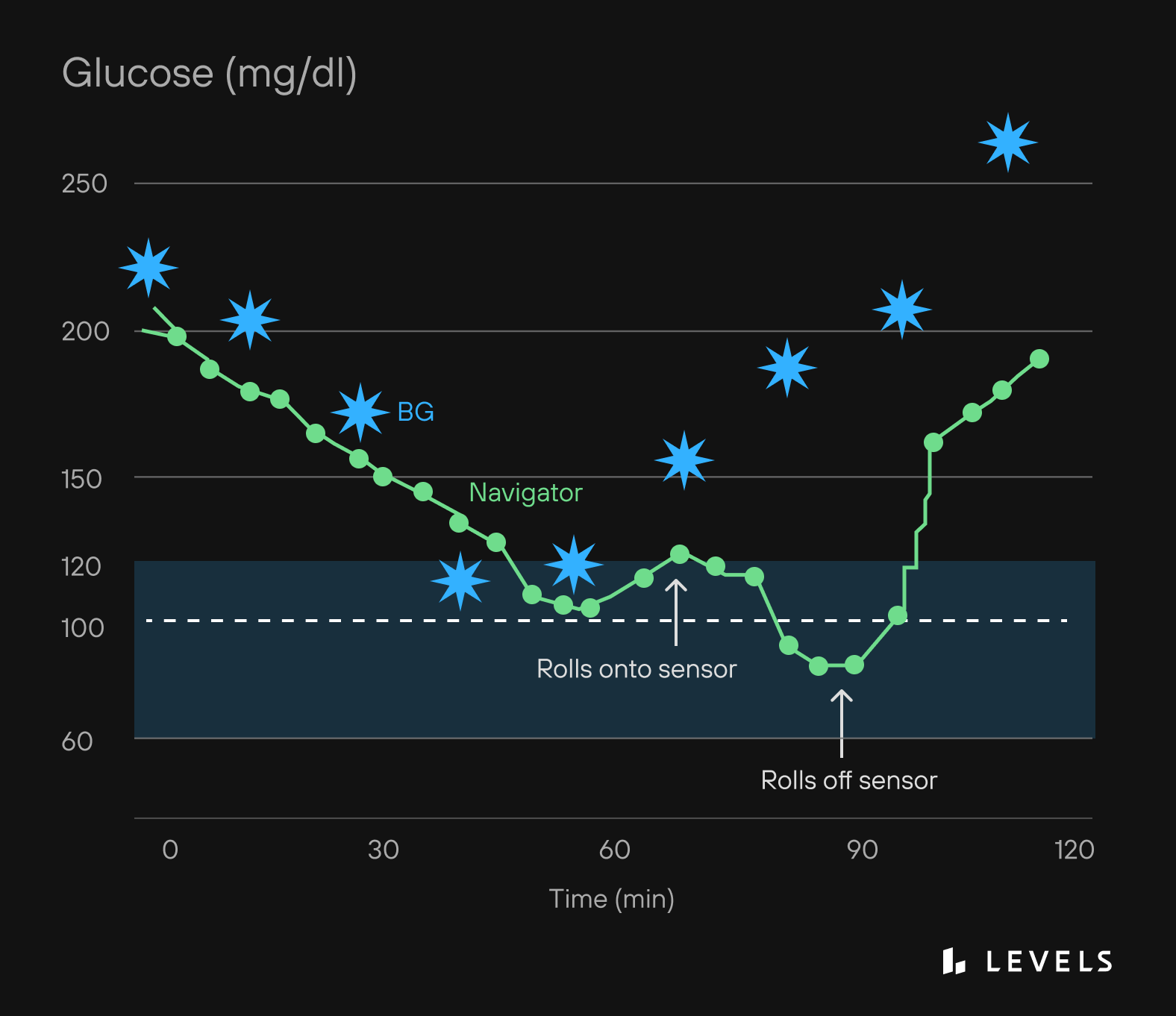
Source: Helton, et al.
Nocturnal Hypoglycemia
In the modern digital world of DIY medicine, a quick Google search may convince you that your glucose dropping at night is a condition called nocturnal hypoglycemia. This condition affects individuals with Type 1 or Type 2 diabetes, is often associated with insulin use, and refers to blood glucose levels dropping below 60-70 mg/dl while sleeping at night.
Nocturnal hypoglycemia most commonly affects diabetic individuals who:
- Skip meals, specifically dinner
- Exercise before going to bed
- Drink alcohol before going to bed
- Have some infection
Some symptoms of nocturnal hypoglycemia include:
- Sweaty, hot, or clammy skin
- Shaking or trembling
- Changes in normal breathing patterns, such as sudden fast or slow breathing
- Higher heartbeat
- Nightmares that wake the person up
If you have a diagnosis of diabetes and have noticed these sudden drops in glucose and experience any of the above symptoms, follow up with a doctor to get a professional opinion.
 Want to learn more about your metabolic health?
Want to learn more about your metabolic health?
Levels, the health tech company behind this blog, helps people improve their metabolic health by showing how food and lifestyle impact your blood sugar, using continuous glucose monitoring (CGM), along with an app that offers personalized guidance and helps you build healthy habits. Click here to learn more about Levels.

 Want to learn more about your metabolic health?
Want to learn more about your metabolic health?






