The most common tool in healthcare for assessing your metabolic health—that is, how well your body processes and uses glucose—is the fasting blood sugar test: your blood sugar uninfluenced by a recent meal. However, measuring what your blood sugar looks like in response to a meal may give you a better glimpse into your metabolic health. That’s called postprandial glucose, and a sharp response is sometimes called a blood sugar or glucose spike. (Postprandial simply means “after eating.”)
Unlike fasting glucose, postprandial blood sugar measurement offers a detailed picture of how your body responds dynamically to food, which can provide an expanded perspective on the state of your underlying metabolic health.
What Is Postprandial Blood Sugar?
Postprandial blood sugar is a measurement of the glucose concentration in your bloodstream in the period up to four hours after eating a meal. When you eat, your body breaks down carbohydrates from foods into simple sugars, glucose and fructose, which absorb into the bloodstream. Glucose is a major fuel source for the body, along with fat. Every cell in your body relies on this energy source to function. In addition to ingesting glucose from food, your body can also make glucose in a process called gluconeogenesis. Your body aims to maintain a consistent level of glucose in your blood, storing or burning excess and making more (or accessing stored supplies) as needed. Having high blood glucose levels is known as hyperglycemia and can put you at higher risk for several health complications.
Insulin is the hormone that helps our cells take in glucose from our bloodstream, bringing our blood sugar back down after a meal. While a sharp rise in glucose is an expected response to a high-carb meal, frequent spikes or glucose that stays high for a prolonged period may be signs that your body has become less efficient at using insulin to remove glucose from the blood. This is called insulin resistance and it’s the root of metabolic dysfunction. Short of measuring insulin itself (usually via a specialized lab test), postprandial blood sugar is the next best window into your body’s glucose and insulin relationship.
Postprandial blood sugar levels too far outside an optimal range can indicate prediabetes or diabetes. Knowing your body’s postprandial blood sugar response is insightful for anyone, but it’s particularly important for those who are pregnant, at risk of diabetes, or actively managing prediabetes or Type 1 or Type 2 diabetes.
 Want to track your postprandial blood sugar?
Want to track your postprandial blood sugar?
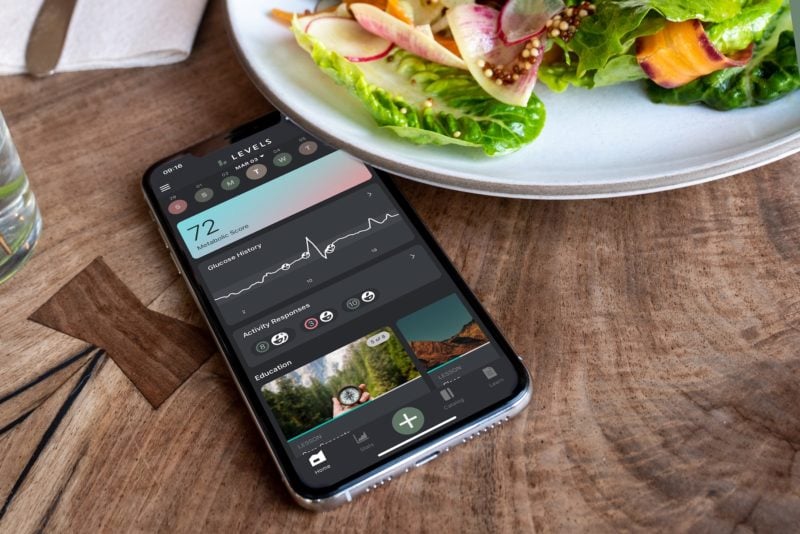
Levels, the health tech company behind this blog, can help you improve your metabolic health by showing how food and lifestyle impact your blood sugar 24/7, including after meals. Get access to the most advanced continuous glucose monitors (CGM), along with an app that offers personalized guidance so you can build healthy, sustainable habits. Click here to learn more about Levels.
What Does “Postprandial” Mean?
When we talk about glucose (or other substances) in relation to food, we can break up our body’s state into three metabolic periods:
- Postprandial: The first four hours after eating or drinking. Complex carbohydrates and simple sugars are absorbed into the bloodstream and lead to an increase in blood glucose. Blood glucose begins rising within a few minutes of eating, but the duration of absorption is around four hours.
- Postabsorptive: This period occurs for about four to six hours following the postprandial period. The liver breaks down glycogen, the stored form of glucose, to keep blood sugar levels relatively stable.
- Fasted: After the postabsorptive period (about 10-12 hours after eating), your body is in a fasted state until your next meal. During this phase, the body produces glucose through non-carbohydrate sources, such as lactate, through a process known as gluconeogenesis. The body also transitions to breaking down fat for energy through the production of ketones.
During the postprandial window, glucose concentrations rise and your body releases insulin to help regulate glucose in the body and store it in a way that can be easily accessed during the postabsorptive and fasting states. If we frequently eat high-carbohydrate meals and snacks, our body can stay in a state of elevated postprandial glucose, requiring the body to regularly release insulin, which can lead to insulin resistance.
Why Postprandial Blood Sugar Matters for Metabolic Health
Poor blood-sugar control can set off a domino effect in the onset of metabolic syndrome. Prolonged elevated blood sugar can lead to insulin resistance and the exhaustion of insulin-producing beta cells, a cardinal feature of Type 2 diabetes. Type 2 diabetes is commonly characterized by a value known as the hemoglobin A1c, or HbA1c. This value measures the percentage of hemoglobin molecules bound to sugar—the more sugar in the blood, the higher the HbA1c will be. It roughly shows an average of your glucose levels over three months (the typical life of a hemoglobin molecule).
A study conducted in France found the loss of postprandial blood sugar control was the first step in metabolic dysfunction and appeared even before elevations in fasting blood sugar. In the study, 130 patients with Type 2 diabetes were placed in five groups according to their HbA1c levels, ranging from under 6.5% to over 9%. Participants used continuous glucose monitors to measure their blood sugar levels over three days as most ate a prescribed diet of 45-50% carbohydrates, 35% fats, and 15-20% protein (participants were prescribed this diet three months ahead of the measuring period and asked to maintain it while wearing the CGMs).
“Postprandial blood sugar can help you understand how your body responds to a specific food or foods.”
The study found elevated postprandial glucose numbers as HbA1c climbed above 6.5%, even as fasting glucose remained normal or near-normal. In groups with higher HbA1c levels, blood glucose levels remained high postprandially and during fasting windows, including overnight.
This data highlights that poor control of postprandial glucose appears to be correlated with worsening metabolic function. This is important for people at risk of diabetes, and also for patients hoping to reverse Type 2 diabetes or prediabetes through diet and lifestyle changes. Monitoring postprandial glucose levels can provide valuable insight into whether insulin sensitivity is improving or if insulin resistance is progressing.
Why Postprandial Blood Sugar Matters If You Don’t Have Diabetes
Avoiding progression to prediabetes or Type 2 diabetes isn’t the only reason to pay attention to postprandial blood glucose. Elevated postprandial blood sugar can also be a predictor of cardiovascular disease mortality and atherosclerosis in people without diabetes—and it’s a better indicator than fasting blood sugar. In fact, in people at greater risk for cardiovascular events, postprandial blood sugar levels are often high even when fasting blood sugar levels are unremarkable.
There are a few reasons for this connection to cardiovascular risk. Frequent episodes of postprandial hyperglycemia lead to the production of free oxygen radicals, which are highly reactive molecules that can damage cells, and in particular, the mitochondria. The mitochondria, the part of the cell that produces energy, can’t keep up with a high metabolic load and generates these free oxygen radicals, which build up over time, eventually overwhelming the body’s antioxidant capabilities, and causing metabolic dysfunction. This is also known as oxidative stress.
In addition, glucose participates in a biological reaction known as glycation, which is when sugar molecules attach to proteins (like hemoglobin). The more sugar that is floating around, the more glycation that occurs. Although glycation is a normal biological reaction, excessive glycation can lead to the damage of blood vessel walls, and can also generate free oxygen radicals. These oxidants have negative consequences for the vascular system, which manifest in inflammation, restricted vessels, and blood clotting—all major risk factors for experiencing a cardiovascular event.
Learn more:
How Postprandial Blood Sugar Affects Your Diet
A one-off blood sugar spike is not cause for alarm (it’s a normal reaction to a carbohydrate-rich meal), but it may lead to a blood sugar crash 2-3 hours after eating, which has its own consequences. In some people, dramatic dips in blood glucose lead to increased hunger and food intake. This was illustrated in a recent study that provided more than 1,000 participants with standardized meals and followed their blood glucose levels using a continuous glucose monitor for 13 days. These people also reported their hunger levels 2-3 hours after each meal.
The people who experienced the largest blood sugar dips reported that they were more hungry 2-3 hours after a standardized meal and chose to eat their subsequent meal sooner (24 minutes earlier on average), compared to people with more modest blood sugar dips. That same group ended up eating an average of 312 more calories as well.
This study suggests that blood glucose levels can influence the brain’s perception of satiety and influence eating patterns.
When Might You Get a Postprandial Blood Sugar Test?
Postprandial blood sugar testing is traditionally recommended for those who are already known to have impaired glucose control. Some scenarios include:
- Elevated fasting blood sugars and/or HbA1c tests may lead your physician to recommend a postprandial blood sugar test to better understand your level of glucose tolerance or to confirm a diabetes diagnosis.
- A person actively managing Type 1 diabetes may undergo a postprandial glucose test to assess whether they’re taking the right amount of insulin after meals and to help prevent potential diabetes complications.
- Pregnant women undergo postprandial glucose testing during weeks 24-28 of pregnancy to screen for gestational diabetes.
Today, it’s also common for healthy people to use postprandial blood sugar tests for nutritional and wellness insights. Postprandial blood sugar can help you understand how your body responds to a specific food or foods. A 2020 study found that there is large variability among people in postprandial glucose response even when they ate the same meal. However, people tended to have the same response to a meal every time they ate it, highlighting the importance of dietary recommendations that cater to a single person versus a one-size fits all approach.
Another useful application of postprandial glucose measurements is for monitoring the impact of lifestyle changes on glucose metabolism. For example, weight loss and exercise can both positively impact postprandial blood sugar levels over time. CGM or time-point-based blood sugar monitoring (usually done with a finger prick and glucometer) can help quantify these changes in your metabolic health.
Postprandial Blood Sugar Tests: How They Work
Postprandial blood glucose tests can be performed using a few methods:
Oral glucose tolerance test (OGTT) is the traditional way postprandial blood sugar tests are performed in medical settings. This is considered the gold standard of postprandial blood sugar tests. During an OGTT, a person is required to drink an intensely flavored beverage that contains 75g of glucose. (The test is done after a period of fasting, so previous meals don’t influence results.) Then they wait, seated and not moving around. A blood sample is typically taken at 30 minutes, 1 hour, and 2 hours after eating, and then plasma glucose is analyzed.
A reading of <140 mg/dL after 2 hours indicates normal glucose response; 140−200 mg/dL after 2 hours would indicate impaired glucose tolerance or prediabetes. Postprandial glucose values above 200 mg/dL meet the criteria for Type 2 diabetes.
Continuous glucose monitor (CGM) testing has the advantages of not requiring a blood sample, and allowing for the easy collection of multiple data points (think: a sample every few minutes rather than once per hour). You can assess postprandial blood sugar in two ways:
- Area under the curve (AUC) analysis. This provides a wealth of information about your body’s glucose tolerance because it measures what scientists call “whole glucose excursion.” Rather than just looking at the peak of a single spike, this essentially captures the whole time your glucose was above fasting levels after a meal, so will take into account how high the excursion was, and how long it stayed elevated. AUC provides a more complete look at postprandial blood sugar levels and has been shown in some cases to be a more sensitive predictor of glucose tolerance and diabetes risk.
- Granular picture of important aspects of glucose response like:
1. How quickly you spiked and returned to baseline
2. How high your peak was, and the delta from baseline to peak
3. Whether you experienced reactive hypoglycemia, or low blood sugar
4. Whether you had a monophasic or biphasic spike (when your blood sugar spikes twice from the same meal)
Glucometers are over-the-counter devices that allow you to measure glucose at home via a small blood sample from a finger prick. You can use them to take measurements at 30 minutes, 1 hour, and 2 hours following a meal.
What is Optimal Postprandial Blood Sugar?
According to the International Diabetes Federation, in a person without diabetes, a postprandial glucose response after a normal meal should not go above 140 mg/dL 1-2 hours after a meal.
It’s important to note that we should aim for even more narrow post-meal levels for optimal health. One study using CGM in people without diagnosed metabolic dysfunction found that the average postprandial glucose peak was 99 mg/dL plus or minus 10.5 mg/dL, far less than the IDF’s recommendation of 140 mg/dL. Another study using CGM in a general population found most people spent 96% of their time between 70 and 140 mg/dL. We recommend trying not to exceed 110 mg/dL postprandial level with no more than 30 mg/dL excursion from fasting glucose. This will ensure that glycemic variability, which is a measure of how “spikey” your glucose is, stays fairly low.
What Impacts Postprandial Blood Sugar Levels?
Postprandial blood sugar responses to the same meal can vary among people. While some of these differences can be chalked up to difficult-to-control factors, like genetics and gut bacteria, other elements are within your control, including:
Macronutrients
Carbohydrates are what drive postprandial glucose levels. Simple carbohydrates like sugar or refined carbs like white flour are likely to cause the most severe spike. Carbohydrates from fiber largely pass through your system undigested and actually help slow the absorption of glucose.
Protein and fat can help lower glucose response because they signal the release of compounds like cholecystokinin, which slow the rate at which food leaves the stomach. Limiting the release of carbohydrates lowers the rate at which blood glucose enters the bloodstream, reducing peak postprandial blood sugar levels.
The order of macronutrients also plays a role in glucose metabolism. Eating protein and fat before the carbohydrates can help blunt a glucose response, which will lead to lower postprandial glucose. In one study, people with normal glucose tolerance, impaired glucose, or Type 2 diabetes ate 50g of cheese and a hardboiled egg 25–30 minutes before taking an oral glucose tolerance test (drinking 75g of glucose). Participants who ate the “preload,” showed lower glucose response than a group that didn’t, and the effect size was greater for those who had greater glucose impairment.
Other Food-Related Factors
Vinegar can also help improve glycemic control and reduce postprandial blood sugar levels. There’s not a clear consensus why, but researchers speculate that it could be because vinegar helps slow the breakdown of carbohydrates and improves our cells’ ability to absorb and use glucose. The type of vinegar doesn’t seem to matter, so use whichever you like: red wine, apple cider, rice wine, or balsamic. (Just keep an eye out for added sugars.) Most studies use 1-1.5 tablespoons of vinegar to achieve the postprandial glucose-lowering effect.
Cinnamon may also help stabilize blood sugar, either by mimicking insulin or increasing its effectiveness. There’s no official recommended dose of cinnamon for people who want to reap its benefits. However, most of the existing research has found effects at doses between one and six grams. Read more about cinnamon’s metabolic effects here.
Sleep
Poor sleep is detrimental to metabolic health and is connected to high blood pressure and obesity. Interestingly, sleep deprivation has been shown to delay the peak release of glucagon-like peptide 1 (GLP1), an intestinal hormone that enhances the release of insulin, following a meal. This may increase the level and duration of postprandial blood sugar elevation. Sleep deprivation also makes us acutely insulin resistant.
Exercise
Exercise is one of the most powerful modulators of blood sugar control. Physical activity stimulates the movement of extra glucose transporters to the surface of muscle cells, allowing for the preferential uptake of blood sugar by our muscles. Exercise is shown to improve postprandial blood sugar levels in both short- and long-term workout programs.
Simply moving more throughout the day also helps. Studies show people exhibit better post-meal glycemic control when they break up long bouts of sitting with less than two minutes of low-to-moderate intensity walking.
Conclusion
Measuring postprandial blood sugar is a proven tool for monitoring our metabolic health. Since no two people eating the same food will experience the same change in blood glucose levels, postprandial blood sugar tests can tell you how your body responds to carbs and your insulin response. Knowing this can help you avoid blood sugar spikes and the potential damage they cause.
 Want to track your postprandial blood sugar?
Want to track your postprandial blood sugar?







