Eating a diet that helps your body make more ketones has become widely popular in the past few years, and for good reasons. Ketones are a natural byproduct of your body burning fat for energy instead of glucose. Optimal metabolic health means your body can switch easily between these two fuel sources—called metabolic flexibility. Research shows that ketone burning may have several health benefits, including reducing inflammation and promoting longevity. Here we look at why metabolic flexibility matters and how you can use a combination of ketone and glucose monitoring to help build your metabolic flexibility.
What is Metabolic Flexibility?
Humans evolved to rely on two kinds of fuel to supply our energy: glucose and fat. During times of abundance, when carbohydrate-rich food is plentiful, the body functions in a primarily glucose-burning mode. If you are metabolically healthy, the glucose you eat either gets delivered from your blood into your body’s cells and used for energy or gets stored as glycogen.
When your circulating and stored glucose is running low during fasting or carbohydrate restriction, your body switches into a primarily fat-burning mode.
“A person with good metabolic flexibility will burn glucose when consuming glucose and burn fat when they consume fat or when their glucose levels run low due to fasting.”
Imagine your body’s energy supply as a fuel tank. At the top of the tank is the glucose circulating in your blood. In the middle is glycogen, the glucose stored in your liver and muscles. At the bottom of the tank are your fat stores.
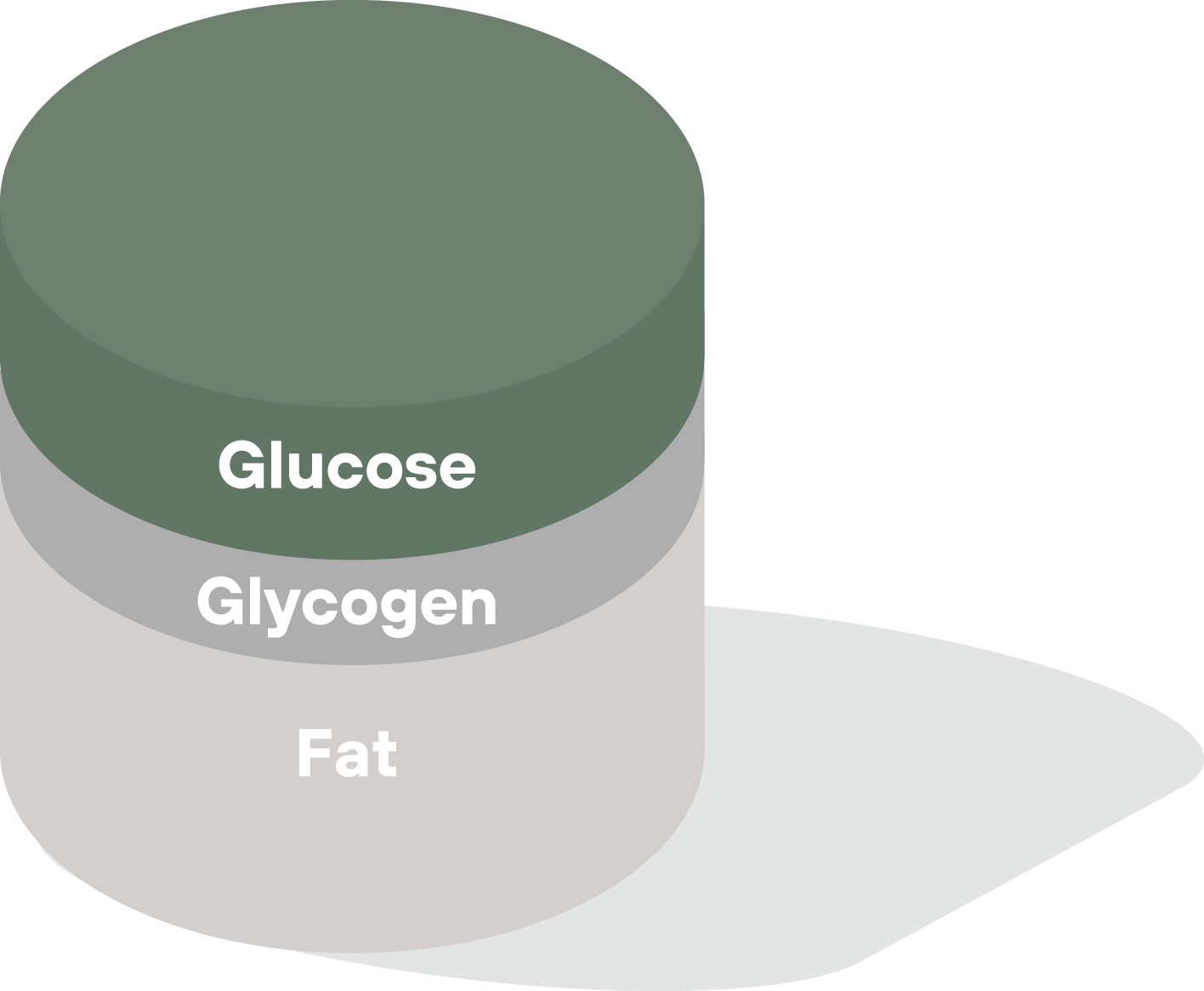
As your body taps its fuel tank for energy, the tank is depleted from the top down. During fasting or carb restriction, the body first burns through excess circulating blood glucose, then its stored glycogen, and finally its stored body fat. (It doesn’t entirely deplete each source—your body will maintain a minimum stable level of circulating glucose—but instead shifts the balance of sources.) When you eat a high-carbohydrate or high sugar meal, your blood sugar levels rise quickly. The glucose is taken up by cells to be used immediately or stored as easy-access glycogen, and any excess is converted to fat for longer-term storage.
Diets high in carbohydrates or sugar remove the need for your body to ever move beyond using the glucose at the top of the tank. Excess glucose starts to pile up in your blood—a state that can lead to obesity, inflammation, organ damage, and a host of metabolic diseases like Type 2 diabetes. By contrast, an eating approach that helps you keep your blood sugar levels in check promotes healthy metabolism—one that efficiently shifts the percentages of the fuel the body is using from glucose and glycogen to fat. If you regularly switch between burning glucose and burning fat, you are said to be metabolically flexible.
Metabolic flexibility refers to how efficiently your body can switch between fuel sources according to their availability. A person with good metabolic flexibility will burn glucose when consuming glucose and burn fat when they consume fat or when their glucose levels run low due to fasting. Metabolic flexibility is thought to be what allows some people to do fasted exercise without running out of energy (since they can tap into fat stores for energy) and eat calorie-dense or high-fat foods without gaining weight. In contrast, metabolically inflexible people may struggle with weight loss, fatigue, or excessive hunger because they cannot efficiently tap into and metabolize their fat stores for energy since their bodies are conditioned to rely on glucose.
It’s important to note that glucose drives the release of insulin, the hormone that helps shuttle glucose into our cells for fuel. One of insulin’s effects is to inhibit fat burning. Therefore, chronically elevated blood sugar and resultant high insulin is a direct inhibitor of metabolic flexibility, putting the brake on fat metabolism. High insulin levels over time can also lead to cells becoming “numb” to insulin’s effects (a state called insulin resistance), which leads to more insulin being produced (called hyperinsulinemia), making the situation worse in a vicious cycle. Ultimately, reducing our exposure to glucose (fasting, minimizing carbohydrates), and finding ways to use the glucose we consume (like exercise), is a big part of solving this problem. By doing this, we reduce our insulin levels, allowing our bodies to utilize fat for fuel, and become metabolically flexible.
As humans, our ultimate strength is our ability to adapt, and our metabolism is part of that superpower. We can exercise our metabolism and improve our metabolic flexibility. Any method of switching between glucose and fat metabolism may help. However, fasting and exercise have shown the most benefit. But how do you know if your efforts are making a difference? That’s where ketones come in.
What Are Ketones?
When your body switches to using fat for fuel, it releases fat from body stores in the form of free fatty acids (FFAs.) Although many tissues in the body can use FFAs for energy, other tissues—most notably the brain—can not. As FFAs are released, your body also creates ketones, an alternate fuel that can be used by the brain and other tissues such as cardiac and skeletal muscle. Essentially, as the body releases fat from storage and FFA concentration increases, so too does the concentration of ketones. Ketones are a biomarker showing your body is burning fat for energy rather than glucose.
But why should you care about raising your ketones? First, elevated ketones are associated with fat loss, improvements in overall body composition (the ratio of lean muscle to fat), and better metabolic health. If you regularly burn fat for fuel instead of glucose, you are less likely to be overweight or obese.
Second, elevated ketones cause the body to turn down its inflammatory response, which may reverse damage caused by, for example, chronically high blood sugar. In addition, there is increasing evidence that raising your ketones may protect against other inflammatory diseases like Alzheimer’s.
Third, elevated ketones likely decrease oxidative stress, which can lead to increased healthspan and longevity.
Fourth, they signify that your body is engaging metabolic pathways that utilize fat for energy and exhibiting metabolic flexibility.
How to Measure Ketones
When we talk about ketones, we’re talking about three different ketone compounds: acetoacetate (AcAc), beta-hydroxybutyrate (BHB), and acetone. AcAc is what your body creates by breaking down fatty acids; BHB is then made from AcAc, and acetone is a side product of that process.
You can test your ketone levels at home in three ways: through the blood, breath, or urine. Blood testing measures BHB and is accurate but is expensive and requires a finger prick. Urine measures AcAc (what is actually metabolized by the mitochondria) but can lose accuracy the longer your ketone levels are raised—also known as a state of ketosis. Breath monitoring is the most convenient and picks up acetone that has moved from the blood into the lungs and excreted in the breath – a direct derivative of AcAc.
Blood or urine ketone measurements are typically in millimoles per liter (mmol/L), and readings can be anywhere from 0 to 6. To know that your body is burning ketones, you want to see a level around 0.5 mmol/L. Breath ketones are measured in parts per million (ppm) or clinical grade ACEs (a proprietary unit from Readout Health) and can be anywhere from 0 to 40 Aces. Levels of 2 ppm or 5 ACEs typically indicate entering ketosis.
According to Dom D’Agostino, PhD, a metabolic researcher at the University of South Florida and Levels advisor, “What’s neat about breath ketones is that it appears to be a better proxy for fat burning in the fasted state, since during prolonged fasting, BHB is quickly swept up by our cells for fuel, thus lowering the amount in the blood. You can see this for yourself when exercising, blood ketones typically drop (as you are using them for energy), but breath ketones rise (as a better reflection of fat-derived ketones). The utility of measuring your ability to burn fat is a representation of your metabolic flexibility.”
What You Can Learn from Monitoring Glucose and Ketones Together
Ketone and glucose monitoring are two sides of the metabolic coin. If we see that our glucose is stable, we can feel fairly confident that our insulin is not being stimulated and know that we have a good shot at unleashing fat burning. We can then confirm that this is occurring by looking at the ketone monitor. If our ketones are not rising in the way we’d expect, we can go back to our glucose monitor and see if we had a rise, which may have prompted the body to release insulin and therefore inhibit fat burning.
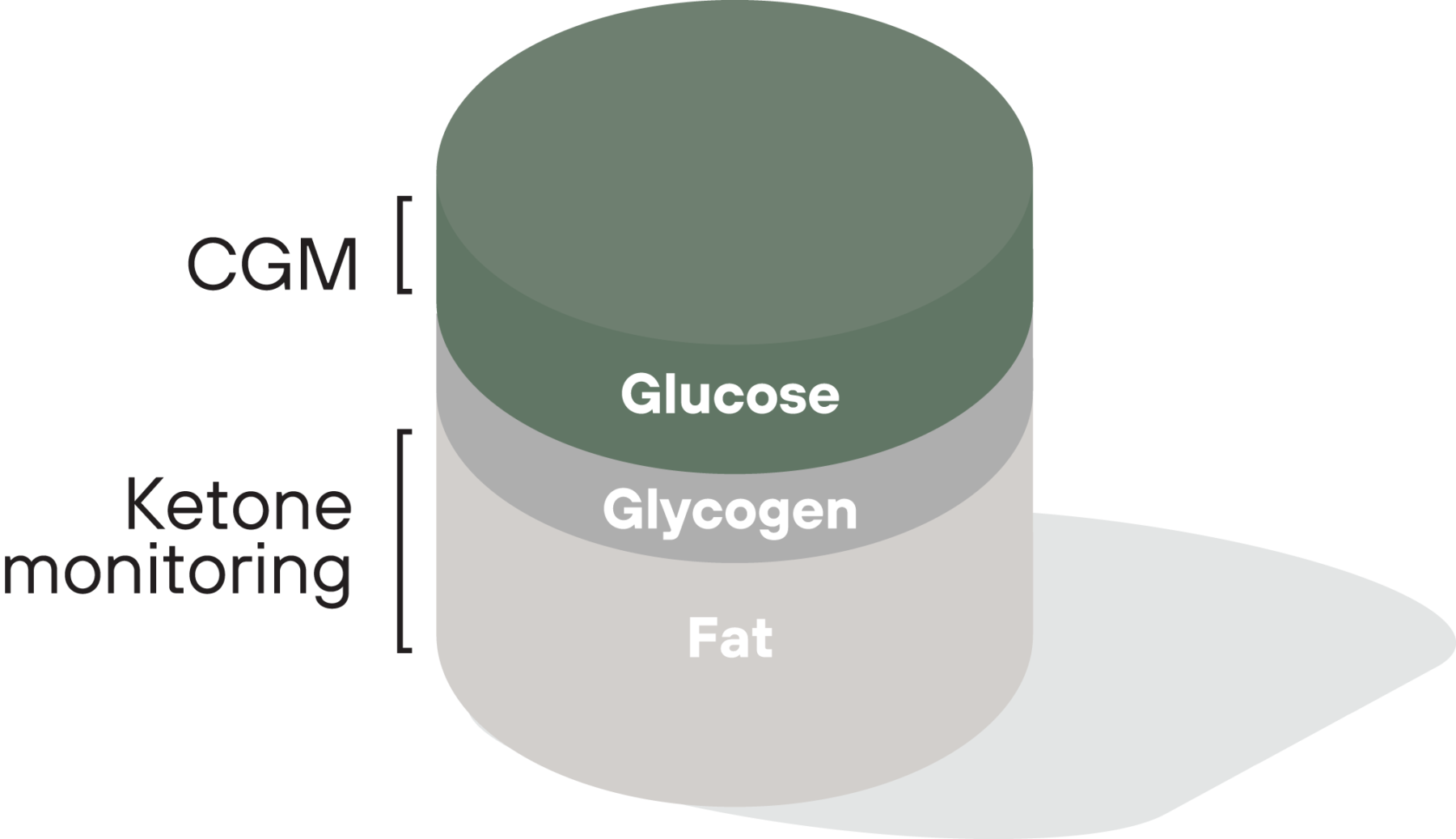
Measuring both glucose and ketones together makes sense as you cannot usually use one measurement to infer the other, mainly because glycogen (which we can’t easily measure) sits in the middle. For example, having low glucose does not necessarily mean you have elevated ketones—your body may be burning stored glycogen instead. Similarly, having low ketones does not mean your glucose is high—even when your glucose is moderate and stable, your body can use it for energy. While continuous glucose monitor (CGM) data indicates when a particular food or way of eating is causing elevated blood glucose, ketone data indicates when exercise or diet leads to glycogen depletion, increased fat metabolism, and the other benefits of ketosis.
For example, you might use CGM to identify and limit or modulate foods that cause your blood glucose to spike. Adding ketone data allows you to see whether these dietary changes are helping you to metabolize fat more efficiently. Keeping your blood sugar in a stable and healthy range over the long term can help lessen the risk of developing conditions related to high glucose, such as diabetes and insulin resistance. Increasing your fat metabolism leads to weight loss, improvements in body composition, and better metabolic health.
Best Uses for Ketone Monitoring and CGM Together
Weight Loss/Intermittent Fasting
One great way to utilize glucose monitoring paired with ketone monitoring is during intermittent fasting (IF). IF simply means adding time between your meals to give your body a chance to use up the glucose you eat and flip the metabolic switch to burning fat for energy. The big challenge is knowing whether your food choices and the length of your fasting period are getting you into a fat-burning state.
While CGM can show you if you are maintaining stable glucose during your feeding period—important so that you don’t go into your fasting period with excess glucose in your system—ketone monitoring can help you see if IF is leading to the goal of fat burning. Used together, these technologies let you optimize and personalize an IF regimen that works best for you. For example, you might find that replacing carbohydrates with protein reduces your blood glucose and reduces the time it takes to begin metabolizing fat.
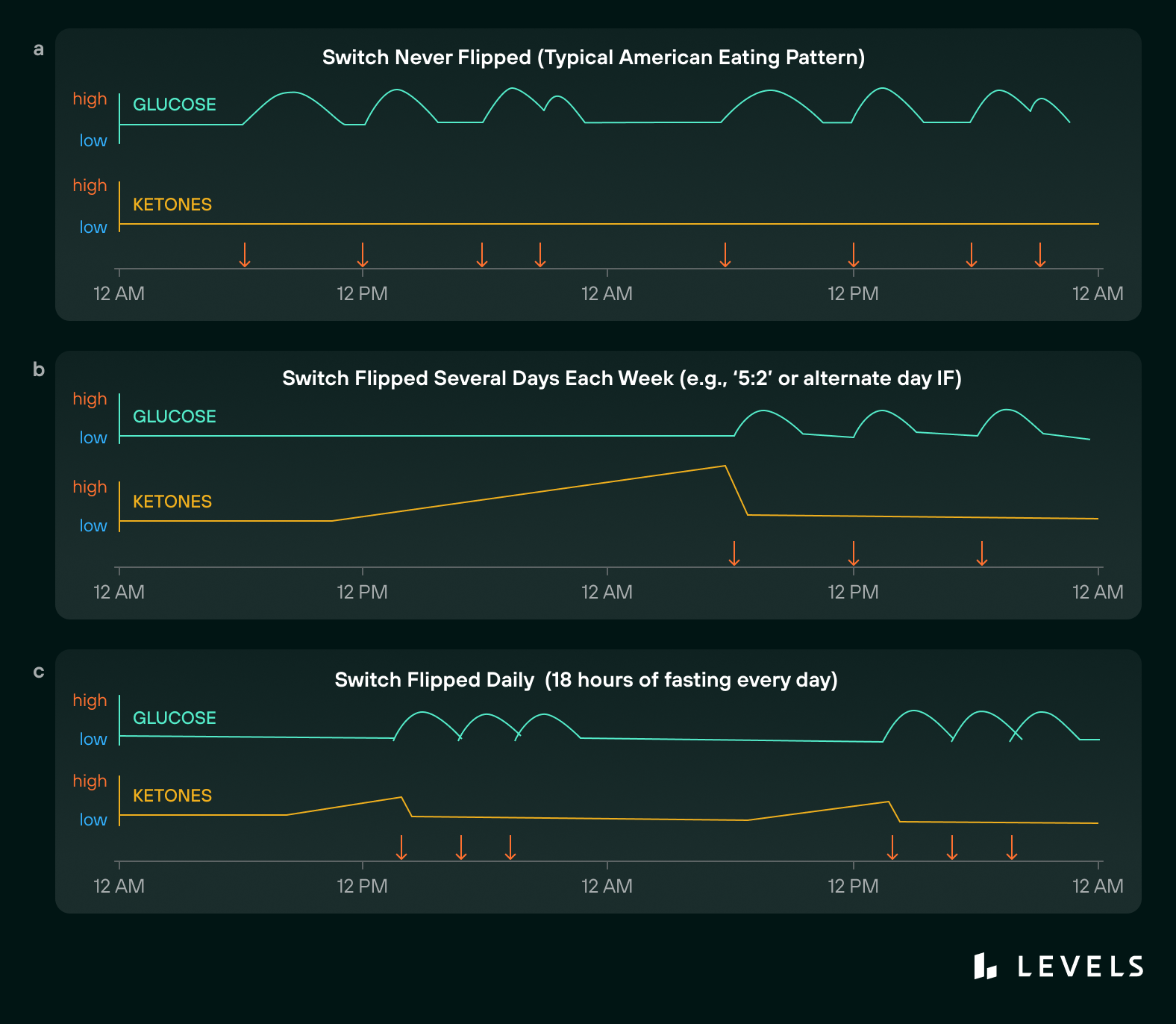
The charts shown below (from this paper) illustrate how different fasting regimes might impact glucose and ketone measurements over a two-day period. (Red arrows represent meals or snacks.)
In the typical American eating pattern of three meals a day plus snacks (a), glucose often remains elevated, and ketones never go up. Low ketones indicate that fat metabolism is sluggish; people eating this way may never flip the switch from glucose to fat burning. The following two charts show how popular IF regimens might work to keep glucose levels in check and increase ketones. In these scenarios, the fasting period is long enough for the body to work through stored glucose and move into fat-burning, raising ketone levels.
Carb-Cycling
CombiningCGM and ketone monitoring can also be a powerful tool for people practicing carb-cycling or refeeding. These regimens use specific eating patterns to allow you to burn carbohydrates during exercise—particularly long or hard workouts—but still increase your fat metabolism. In this case, CGM can reveal how your fueling choices impact your glucose levels, so you can see what’s available to your body on intense training days. On lighter days, ketone monitoring can let you know if you’re successfully metabolizing fat. Together, CGM and ketone data can help you build your personalized carb-cycling protocol.
Used together, CGM data and ketone data provide a granular view of what fuel you are burning and its level in the body in real-time, allowing you to tailor your diet and exercise to improve metabolic flexibility.
Readout Health authored this article with editorial oversight by Levels. Readout Health is a digital biomarker company that provides full-day ketosis trends and insights through its patented breath technology. Thousands of consumers and patients use Readout’s handheld BIOSENSE device for an accurate indication of their ketone levels from a simple breath. Backed by a 2019 clinical trial that exposed the high variability of ketones throughout the day, BIOSENSE replaces finger pricks with frictionless and frequent testing to reveal which foods kick you out of the fat burn state. The companion app personalizes fasting regimens, carb restrictive protocols, and clinical programs in disease prevention and reversal.