What Alcohol Does to Glucose Levels
Rates of obesity and lifestyle-related chronic disease are soaring, and we are continually reminded of the importance of being vigilant about how we live and eat. Interestingly, many symptoms and diseases that slow us down are rooted in metabolic dysfunction and the body’s compromised ability to efficiently process glucose (the sugar our cells use for energy). It seems that the way we live, eat, and drink has collectively gummed up the system for many of us, making us sicker, more tired, and less fit than ever.
Read on to gain insights into the relationship between alcohol and metabolic fitness.
I Just Had a Drink: What’s Going to Happen?
The effects of alcohol on blood sugar depend on several factors, such as whether you’ve eaten recently, are fasting, or are in a ketogenic state. These effects are also influenced by whether you mix the alcohol with other carbohydrate-containing liquids like juice or soda.
Under normal conditions, the liver makes glucose from chemical building blocks like lactate, alanine, and glycerol in a process called gluconeogenesis. The liver also breaks down stored chains of glucose in it through glycogenolysis. Both of these processes are intended to release glucose into the blood to provide energy to our brain and muscles and prevent hypoglycemia, a sometimes dangerous state when glucose levels are too low. The body regulates these processes well and keeps glucose levels in a reasonably narrow range under normal, healthy conditions.
It’s thought that drinking alcohol decreases the liver’s ability to make new glucose via gluconeogenesis, which can lead to lower circulating glucose levels. To counter this decrease, alcohol stimulates the breakdown and release of stored glucose. This balance between impaired gluconeogenesis and increased glycogenolysis means acute alcohol intake shouldn’t significantly affect glucose levels for normal, healthy people eating a standard diet.
However, the situation is different for those who’ve been fasting or are in a ketogenic state because these people already have much less glucose stored as glycogen in the liver and muscles. Usually this state prompts the liver to produce new glucose via gluconeogenesis, but, as noted above, alcohol inhibits this process. The result is that glucose levels can fall to dangerously low levels, and in extreme cases, without treatment, this hypoglycemic state can lead to seizures, coma, or death.
What About Having Alcohol With A Meal?
A study involving healthy, lean people showed that consuming a small amount of alcohol (20 grams or about 1.5 drinks) one hour before a carbohydrate-rich meal can lead to significantly lower post-meal glucose and, for some types of alcohol, insulin levels than if that same meal were eaten without alcohol. The effect of drinking alcohol before or during the meal ranged from a 16% to 37% reduction in post-meal glucose.
So why is this happening? We’re already familiar with how alcohol inhibits the production of new glucose, which is part of the puzzle, but light-to-moderate alcohol consumption could also cause an acute increase in insulin sensitivity (insulin sensitivity and resistance refer to the efficiency with which the body can use insulin to store or burn glucose), which would lead to more rapid uptake of sugar from the meal into the cells. It’s important to note that the effect of alcohol consumption on insulin sensitivity is controversial, with studies showing variable findings.
Long-Term, Heavy Alcohol Use
Chronic, heavy alcohol use can cause alcoholic liver disease (ALD) and damage insulin-producing pancreatic beta cells, both of which lead to glycemic dysregulation. It’s known that people with ALD have a higher risk for Type 2 diabetes, even compared to people who have advanced liver disease from other non-alcohol-related causes, such as hepatitis.
These problems are likely due to a combination of effects, including impaired insulin secretion from the pancreas, reduced tissue responsiveness to insulin, and a decreased ability to store glucose as glycogen. Heavy alcohol use is also thought to impair insulin receptor signaling, making the entire body more resistant to taking up glucose into cells. Pancreatic beta cells are particularly sensitive to the toxic cellular effects of acetaldehyde, a metabolite of alcohol.
Binge Drinking
Binge drinking—defined as 5 alcoholic drinks within 2 hours for men or 4 alcoholic beverages within 2 hours for women, even just once a month—is associated with an increased risk of Type 2 diabetes. Binge drinking also acutely increases inflammation in the body and brain and can disrupt neural control of metabolism, generating whole-body insulin resistance. These impairments can persist even after the alcohol has been metabolized.
In a study in rats, binge drinking the equivalent of seven ounces of alcohol for three consecutive days leads to a state of rapid insulin resistance. This insulin resistance can last for more than two days after the last drink is consumed. Under normal circumstances, the brain can send signals to the liver (an organ intimately involved in glucose regulation) about when to break down, make, or store glucose. However, in the setting of binge drinking, this conversation between the liver and brain is impaired. In the rats in this study, binge drinking seemed to specifically cause inflammation in the brain, which blocks the brain from receiving proper signals from circulating insulin and increases the expression of a protein that negatively regulates insulin’s effect in the brain.
Does binge drinking affect men and women in the same way in terms of metabolic health? The answer appears to be no, and women tend to fare worse. A study of 897 people assessed fasting plasma glucose levels and drinking habits from age 16 to 43. This long-term data showed that total alcohol consumption combined with binge drinking behaviors between these ages was associated with disproportionately elevated fasting glucose in women at age 43. Interestingly, these results were independent of BMI, meaning that it was unlikely elevated weight was causing the higher fasting glucose in heavy drinkers.
Moderate Alcohol Consumption
Compared to heavy drinkers or those who abstain entirely, people who consume moderate levels of alcohol seem to have a lower risk of Type 2 diabetes and higher insulin sensitivity, although the reasons why aren’t fully clear yet. It may be related to the fact that alcohol consumption seems to increase the body’s adiponectin levels, a protein with anti-diabetic and anti-inflammatory effects.
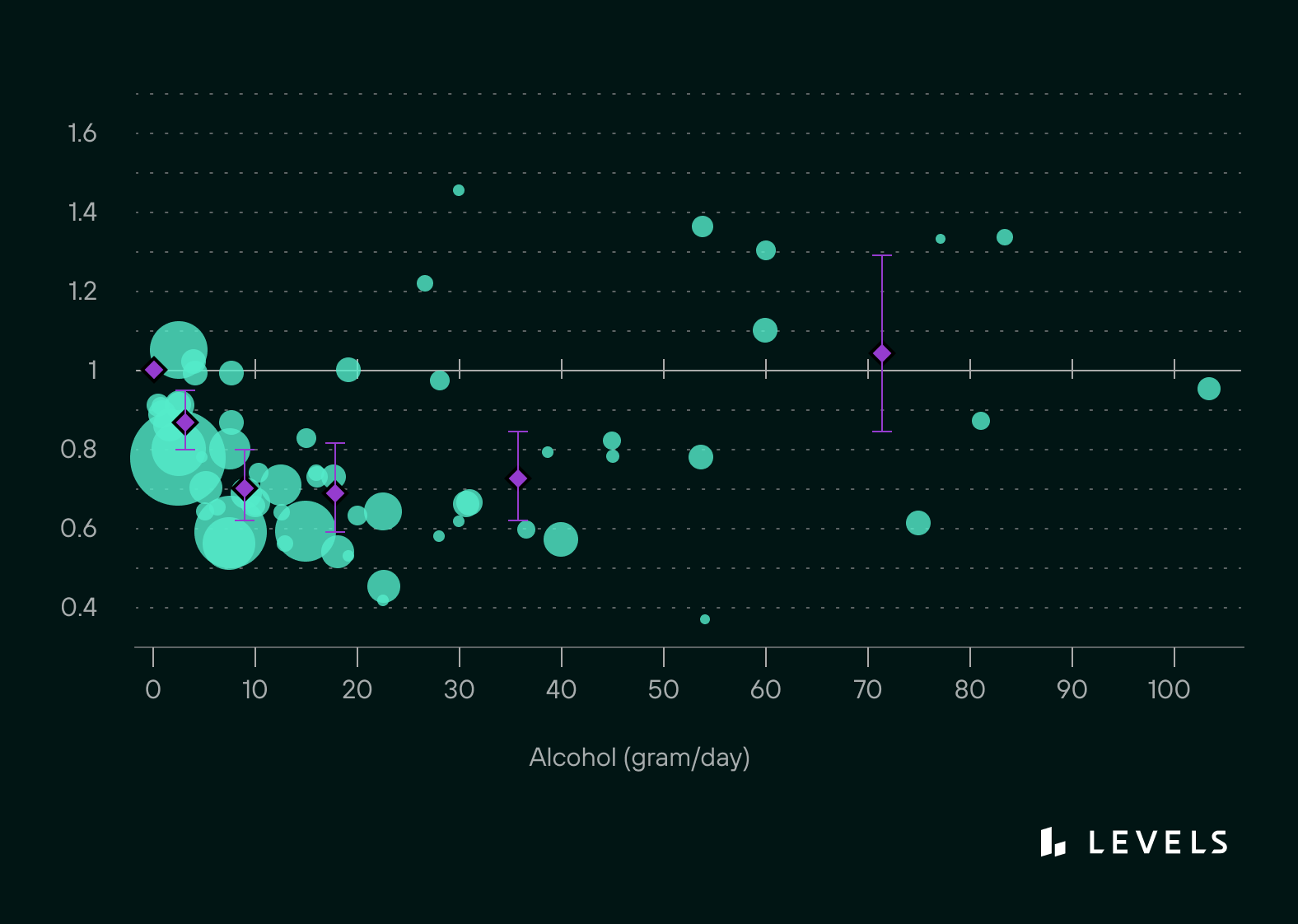
Compared to heavy drinkers or those who abstain entirely, people who consume moderate amounts of alcohol have a lower risk of Type 2 diabetes and higher insulin sensitivity. A large meta-analysis, compiling data from 14 studies on the metabolic effects of moderate alcohol consumption, showed decreased hemoglobin A1c and fasting insulin levels. Additionally, in a study of 360,000 people followed for an average of 12 years, there was a 30% reduction in new-onset diabetes in people who consumed 1-2 drinks per day. In much of the research, there appears to be a “J-shaped curve” relating alcohol consumption and diabetes risk: Those completely abstaining had a slightly higher risk than those drinking a light-to-moderate amount, while the heaviest drinkers were at the highest risk.