The Paper
Women: Diet, Cardiometabolic Health, and Functional Medicine
Author: Sara Gottfried, MD, Director of Precision Medicine at the Marcus Institute of Integrative Health at Thomas Jefferson University
Published: May 2022
The Takeaway:
Women have a higher risk of cardiometabolic disease than is often known or acknowledged, leading to gaps in treatment and diagnosis. A functional medicine, root-cause approach can help address some of these gaps.
What It Looked At
The article goes through differences in both physiology and outcomes that impact women and cardiometabolic disease, which is the leading killer in women as well as men (in fact, women have higher cardiometabolic mortality than men), though less than half of women know it (and doctors are not much more informed). Furthermore, reductions in mortality from innovations over the past few decades have benefitted men far more than women. Cardiometabolic disease includes coronary heart disease, heart failure, diabetes, breast cancer, and Alzheimer’s. Gottfried details the functional medicine approach to diagnosing and treating patients, looking at antecedents, triggers, and mediators.
“Half of the women in developed countries will die of mostly preventable heart disease or stroke, and one woman dies of cardiovascular disease every 80 seconds in the United States.”
Antecedents are genetic and gene expression factors that influence health. Triggers are events that contribute to or initiate disease, such as pregnancy, trauma, or menopause. Mediators are habits or other external conditions, such as smoking or toxin exposure.
Gottfried also explains seven physiological factors that influence health, including the microbiome, glucose regulation, immune response, and hormone signaling.
Finally, the paper examines several functional medicine treatments, such as additional biomarker testing, lifestyle interventions, and hormone therapy.
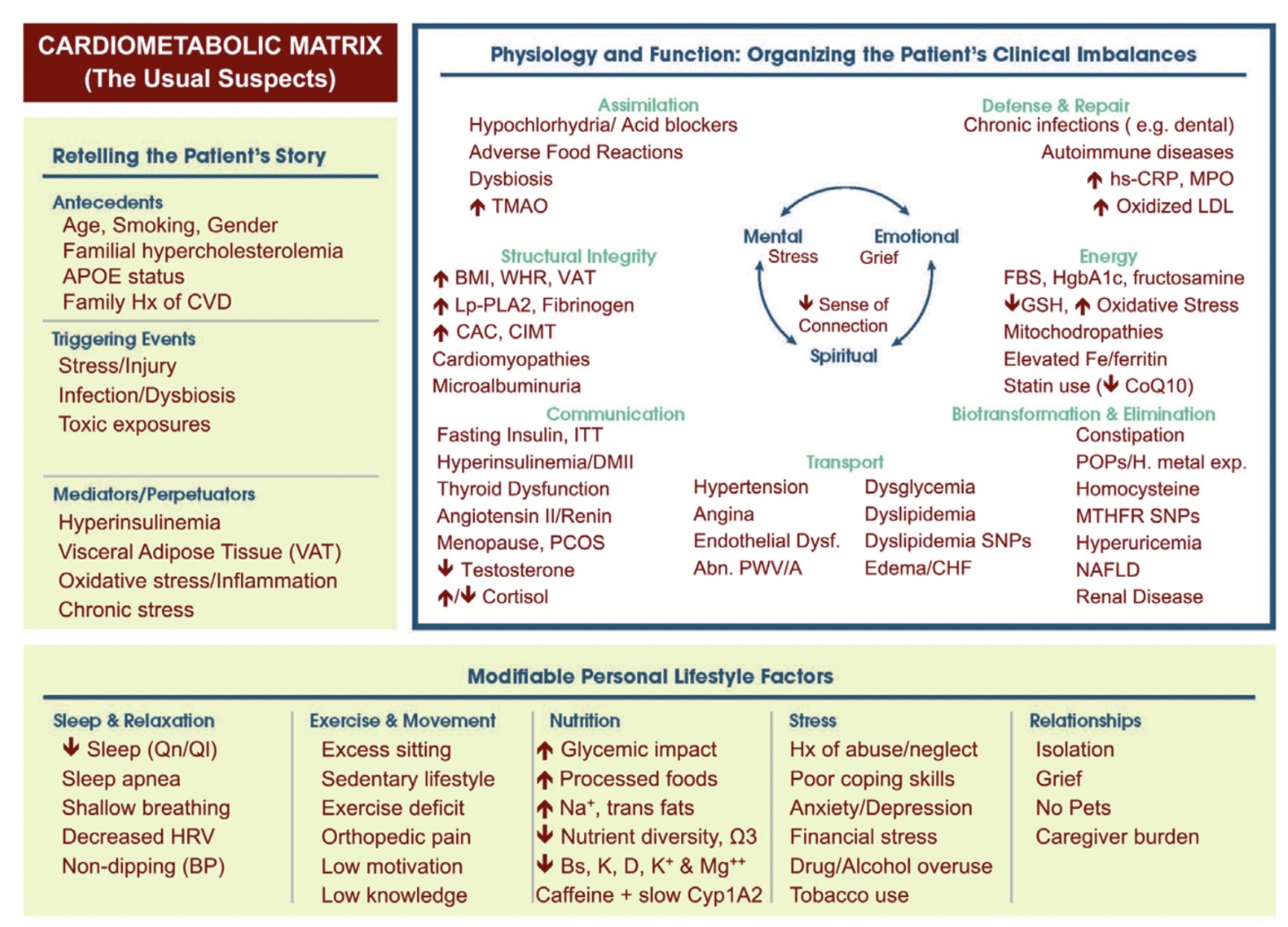
Cardiometabolic Matrix from the Institute for Functional Medicine. (Used with permission from The Institute for Functional Medicine (IFM), the global leader in Functional Medicine and a collaborator in the transformation of healthcare.)
What It Found
The statistics around women and cardiometabolic disease are sobering.
- Half of the women in developed countries will die of mostly preventable heart disease or stroke.
- One woman dies of cardiovascular disease every 80 seconds in the United States.
- Women account for two-thirds of cases of Alzheimer’s disease
- Women have a higher prevalence of autoimmune disease
And although some of the risk factors for disease are the same among men and women—hypertension, smoking, poor cholesterol—some, such as smoking and insulin resistance, can be more damaging in women. (Smoking, for instance, leads to a 25% higher risk of coronary heart disease in women.) In addition, women face many unique risk factors, including polycystic ovary syndrome (PCOS), pregnancy, perimenopause, and menopause. (For example, gestational diabetes increases Type 2 diabetes fourfold.)
Many of the traditional healthcare systems are not addressing these gaps:
- Women are underrepresented in clinical trials.
- “Less than half of physicians said cardiovascular is a top concern for women along with breast health and weight.”
- “Women experience delays in receiving care, poorer outcomes when treated by male physicians, and lower rates of guideline-based medical therapy than men.”
In the second half of the paper, Gottfried offers a framework that can help address these inadequacies in a functional medicine approach. Functional medicine is a systems-based method of care that tries to identify the root causes of illness in how different parts of the body interact and address those causes with upstream interventions. By contrast, traditional medicine often treats each problem as unique and handles it with an acute treatment like a pill or surgery (though functional medicine does not preclude those interventions).
Gottfried lays out a matrix of factors influencing disease, symptoms and conditions, and interventions. Looking at health in this more comprehensive view can help clinicians identify those unique risk factors for women and individual patients. For example, women appear to have a higher risk of cardiometabolic disease than men both from genetics and hormonal changes associated with menopause—these are known as antecedents. A patient may also have trauma in their childhood or multiple pregnancies (triggers), both of which increase disease risk.
In the Clinical Imbalances section of the matrix, we see how these gender differences manifest in physiological markers. For example, women face higher coronary risk at lower glucose thresholds than men. Hypertension reduces lifespan more for women over 50 than men. Women even get more antibiotic prescriptions, which impacts their microbiome health.
Finally, Gottfried details how functional medicine attempts to address these differences through more comprehensive testing, including stress perfusion cardiac magnetic resonance imaging, which can pick up more subtle changes in vascular function more likely to manifest in women. She also walks through common functional medicine treatments, including nutrition (often centered around a Mediterranean Diet), microbiome intervention, and hormone therapy.
Why It Matters
Mainstream medicine is failing to catch early signals of disease when lifestyle interventions have a greater chance of reducing risk. This is true across gender, but Gottfried’s paper points out the many ways that the cardiometabolic deck is stacked against women. As she says in the conclusion, “We need to challenge the dogma that women are at lesser risk of cardiometabolic disease than men, or that their risk does not begin until they are 10 years or longer from menopause. We need to understand sex-based differences in chronic disease and in medical research and translate our understanding of these differences into clinical practice.”
The best way to address these challenges is to make more women aware of their unique risks, especially with regard to nontraditional risk factors for coronary heart disease and baseline metabolic health, and to make clinicians more aware of approaches to identify and treat disease early.








