Our metabolic health is a result of so much more than our dietary and exercise habits. Metabolism is the collective chemical reactions by which our cells churn food into fuel to power our bodies. While we may think of the process as merely physiological, it’s also tied to our psychology and history. Early life trauma—which is quite prevalent—and repeated stress over time can both be detrimental to our metabolic health. And we may even pass the effects down for generations.
The link between chronic stress and poor metabolic health is well-established. However, researchers are still trying to understand the exact mechanisms and pathways of how early traumatic experiences can impact metabolic health immediately and in the long term. But the link is there. They know that heightened stress processes at a young age can alter our physiology. Evidence points to the ways in which trauma gets “biologically embedded.” Coping mechanisms, in the form of unfavorable lifestyle habits, also come into play.
“Excessive challenges to the brain and exposure to profound stress may exhaust our stress, metabolic, and immune response systems,” explains Jagdish Khubchandani, PhD, a professor of public health at New Mexico State University. “Later, after multiple or profound stressors, we are not able to deal with stress properly, or the abnormal stress response can cause diseases. Cortisol, a hormone that regulates response to stress by the immune, metabolic, and inflammatory pathways, gets dysregulated, causing disease.”

Childhood Trauma and Poor Metabolic Health
What are Adverse Childhood Experiences?
Adverse childhood experiences (ACEs) are potentially traumatic events before age 18. ACEs include violence, physical and emotional neglect, all forms of abuse, and household dysfunction, according to the Centers for Disease Control and Prevention (CDC). Household dysfunction may include divorce; intimate partner violence; or having a loved one who is incarcerated, dealing with substance use disorder, or struggling with mental health issues.
A 1998 CDC and Kaiser Permanente study published in the American Journal of Preventive outlines these specific ACEs. But the CDC states that the list is by no means exhaustive. The American Academy of Family Physicians, for example, also lists bullying, crime, the sudden loss of someone close, severe illness, natural disasters, life-threatening accidents, crime, kidnapping, and war.
ACEs sometimes coincide with another set of ACEs known as adverse community environments. Examples include growing up in poverty, facing systemic discrimination, or residing in a violent neighborhood, according to the National Conference of State Legislatures (NCSL).
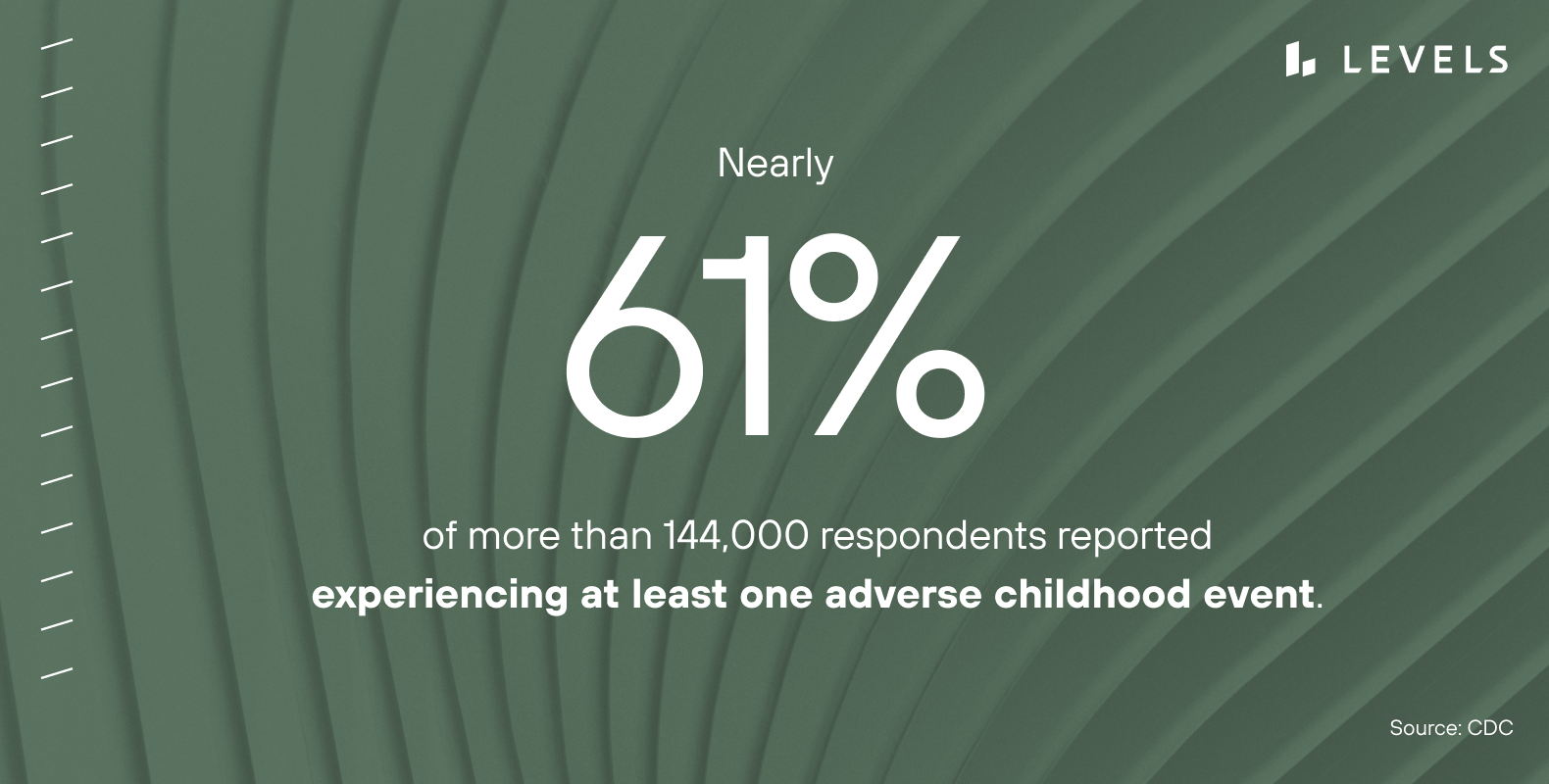
A CDC study published in 2019 shows ACEs are quite common. The researchers used Behavioral Risk Factor Surveillance System (BRFSS) data from 25 states. Nearly 61 percent of the more than 144,000 respondents reported experiencing at least one ACE, while almost 16 percent reported exposure to four or more.
Childhood Adversity and Chronic Health Conditions
“Childhood is a critical period in an individual’s life when they need nurturing for the mind and body,” says Khubchandani, who has researched the association of ACEs and migraine in women. “A lot of transitions occur in this phase, along with the development of organs, processes, and thoughts.” He adds that when we face adversity during this period, it can have a lasting impact.
In the 2019 CDC research, adults in the study with the highest level of ACEs had a greater odds of having chronic health conditions when compared to those with no ACEs. For example, they had a 20 percent chance of being overweight or obese.
A study in New Zealand published in JAMA Pediatrics in 2009 assessed health data for more than 1,000 32-year-olds. Those with ACE exposure had a greater risk of high inflammation levels and metabolic risk biomarkers, including high cholesterol and high blood pressure, as well as an increased risk for age-related diseases when compared to those who did not experience childhood trauma. And a 2021 New Zealand study analyzing 2,888 survey participants showed that those with higher ACE exposure had an increased likelihood of reporting mental health issues, disability, and chronic health conditions, including heart disease and diabetes.
A 2014 study published in the journal Social Science & Medicine looked more specifically at whether ACEs impact the risk of developing metabolic syndrome. Metabolic syndrome is a group of conditions—high waist circumference, high fasting blood sugar, low HDL, high triglycerides, and high blood pressure—that increase one’s risk of heart disease, stroke, and Type 2 diabetes. Biomarker and questionnaire data for 1,200 people showed that those who experienced moderate to severe childhood trauma had more of the five metabolic syndrome symptoms than people with no abuse. And ACE exposure increased their risk for having metabolic syndrome diagnosis, meaning they had at least three of the symptoms.
Childhood Adversity and Pathways to Poor Metabolic Health
The epidemiological link between ACEs and disease risk is well established. But researchers are still learning about the pathways that may lead to adverse health outcomes like metabolic dysfunction after childhood trauma. Likely several factors are involved.
ACEs flood the brain with the stress hormone cortisol and inflammatory cytokines that then hinder neural development in regions responsible for stress regulation, according to a 2017 review published in BMC Medicine. Researchers refer to this concept as the “neurotoxicity hypothesis.” And the 2019 CDC study also states that these “toxic stress responses” have an immediate physiological impact.
A 2014 review published in the journal Child and Adolescent Psychiatric Clinics of North America takes a closer look at some of these processes. The review reports that each time we experience an ACE, it triggers our sympathetic nervous system’s fight-or-flight-or-freeze response. Our hypothalamus releases corticotrophin-releasing hormone (CRH), which stimulates the release of adrenocorticotropic hormone (ACTH), which leads to cortisol release. After children face early trauma, whether one event or a series of experiences, their CRH levels remain elevated into adulthood, and their baseline cortisol levels may be somewhat altered. According to the review, studies show that people who’ve experienced ACEs might also then be primed with a heightened stress response when facing future stressors or triggers. That fight-or-flight switch gets triggered more quickly and with more intensity, meaning they may have a bigger flood of cortisol compared to someone who hasn’t experienced childhood adversity. In some cases, the fight-or-flight switch may never truly get shut off, leaving someone in a state of hypervigilance, where they are always subconsciously assessing danger. Early trauma may also dysregulate the neurotransmitter serotonin, which is critical for feelings of well-being. Decreased levels are associated with depression and anxiety.
In addition to driving stress and inflammatory processes within the body, ACEs might impact brain signals that tell us when we’re hungry or sated. Trauma possibly triggers excess signaling of catabolic hormones—such as cortisol, epinephrine, norepinephrine, and glucagon. Over time, this excess signaling can impact metabolic health. Excess cortisol, for example, appears to elevate blood sugar, which can eventually make cells insulin resistant.
Interestingly, researchers of a small 2021 study published in Molecular Psychiatry say childhood trauma may “act as a ‘first hit’ with the appearance of insulin resistance.” And that severe adulthood stress “could represent a ‘second hit,’ which could lead to an even more dysfunctional metabolic response.” Their preliminary study looks at glucose metabolism biomarkers in 72 adults. The biomarker levels differed whether the study participants experienced childhood trauma, severe adulthood events, both, or neither. People exposed to both childhood trauma and stressful experiences later in life had the highest levels of biomarkers.
Childhood Adversity and Genetics
We may also pass down physiological changes resulting from childhood trauma from generation to generation. A small 2020 study examined how early trauma affects the metabolic pathway at the genetic level. In the two-part study, male rodents separated from their mothers and exposed to early life stress exhibited metabolic dysfunctions. The dysfunctions were specifically related to their metabolism of some polyunsaturated fatty acids (PUFAs), and the result ultimately affected the production of steroid hormones. These same dysfunctions were later present in their offspring, and the issue continued for generations of mice.
Next, blood and saliva samples collected from 25 children—ages 6 to 12, all living in the same orphanage—showed the same metabolic dysfunction biomarkers as each other and the mice. The issues were not present in a control group of children who hadn’t experienced ACEs. After further research with mice, the researchers note that changes in PUFA metabolism after exposure to ACEs alter a type of hormone receptor that affects gene expression and DNA, especially in sperm cells. Ultimately, sperm carry the metabolic dysfunction on to the next generation.

Childhood Adversity and Lifestyle Habits
Poor metabolic health or metabolic dysfunction may also occur by way of the coping mechanisms people might adopt after exposure to childhood trauma.
“My opinion is that disease processes are influenced by physiological processes and behavioral responses to ACEs,” Khubchandani says. “ACEs get biologically embedded, and social and policy factors can affect how negatively ACEs can influence our biology and physiology.”
A 2019 longitudinal survey published in the journal BMC Public Health examines the relationship between ACEs and adult-onset Type 2 diabetes. The researchers also explore the role of “risky health behaviors,” such as smoking, heavy drinking, and obesity. Around 10 percent of the more than 8,000 study participants developed diabetes between ages 18 and 52. For men, more than four ACEs were associated with diabetes, but not individual adverse events. ACEs were also associated with daily smoking and being underweight for men. For women, two or more ACEs were associated with the likelihood of developing diabetes, and trauma was also associated with smoking and obesity.
ACEs are also a risk factor for substance use disorder, which can contribute to poor health, according to a 2010 study in Addictive Behaviors. The research looks at data for a little over 2,500 people. Those with more exposure to ACEs were more likely to depend on alcohol, cocaine, or opioids. Those who grew up in households where substance abuse occurred had a two-thirds greater risk of substance abuse as an adult. The researchers point out that substance dependence can have a genetic component, which could be a possible relationship. But the association between ACEs and substance use disorder was higher for those with mood or anxiety disorders. Therefore, the researchers say mental health issues, potentially brought on by childhood trauma, could be what’s causing the increased risk for substance abuse.
Research that links ACEs to metabolic syndrome also shows how lifestyle factors contribute. For example, sleep problems increase the association between ACE exposure and metabolic syndrome. Plus, poor sleep quality is associated with overeating, depression, and alcohol consumption. But more studies are needed to explore how lifestyle might further exacerbate the detrimental physiological effects of ACEs and how altering habits and coping strategies may help.
“Working with a trauma-informed therapist can significantly impact the health trajectory,” says Liza R. Clancy, DBH, LCSW, who has studied the health impact of ACEs and whose specialty as a psychotherapist is helping patients understand how they are wired in response to early environmental and developmental trauma. “By attuning with the therapist to explore what happened and its impact,” she explains, “the patient can begin to understand his or her behavior as a coping mechanism, leading to self-acceptance.”
What About Everyday Chronic Stress and Metabolic Health?
In the face of a quick stressor, such as narrowly avoiding a fender bender or having to give a presentation, our heart rate quickens, and other fight-or-flight responses kick in. The physiology occurs along the hypothalamic-pituitary-adrenal axis, impacting various hormones and setting off all the necessary chain reactions. They’re our body’s way of quickly adapting to the perceived threat we’re facing. But when we realize everything is fine, our body returns to its baseline state a few minutes later.
Most of us regularly face a handful of minor stressors or general daily life juggles. And our bodies were built to manage them. But all of us at one time or another face bigger traumas or even periods of chronic stress, the loss of a loved one, for example. Even if you haven’t experienced childhood adversity, stress in adulthood can pile up and affect your metabolic health.
When traumas add up throughout childhood or in our adult lives, or we live in a state of chronic stress, we can experience what’s called allostatic load or overload. Essentially, all that adapting and readying for a threat comes at a cost physically and mentally. Our fight-or-flight responses are meant to help us endure and survive during a moment of high stress. We need cortisol and adrenaline to, say, fight off an attacker or to finish the last grueling miles of a marathon. But these responses are only helpful in the short term. In the long-term, the hormone rush and other stress processes, like elevated blood pressure and a high heart rate, have damaging effects.
Plus, the “fight or flight” response of our sympathetic nervous system acts, in some ways, in direct contrast to the “rest and digest” response of our parasympathetic nervous system. We need our parasympathetic nervous system to activate so we can relax. But when we’re constantly activating our sympathetic nervous system because of stressor after stressor, our stress response remains primed. Our cortisol levels stay high, and we have a more challenging time flipping the switch to a calmer state.
Indeed, a 2021 review published in Psychotherapy and Psychosomatics reports that ACEs and chronic stress are linked to high levels of allostatic load in adulthood. And allostatic load is associated with metabolic syndrome, heart disease, and Type 2 diabetes. The review found that poor sleep quality, poor diet, being overweight, alcohol consumption, and smoking are associated with a higher allostatic load. But exercise is associated with lower levels. The researchers theorize that stress management tools and strategies that promote well-being may help lessen the cumulative effects of repeatedly facing intense situations.
What Can Be Done About ACEs or Chronic Stress?
Just because you have chronic stress now or were exposed to childhood trauma does not mean poor metabolic health is in your future.
Clancy says people invested in their health can often achieve better outcomes. What they sometimes need are new tools. “Cognitive-behavioral interventions are useful in learning skills to retrain maladaptive responses,” she explains. “Mindfulness is key in helping patients to self-regulate and manage stressors and can have a significant impact on health conditions and psychological well-being.” Mindfulness methods might include meditation, breathing exercises, yoga, other forms of movement, or anything that helps someone regain a sense of calm.
Research published in the journal Nutrients shows that people with depressive symptoms who engaged in mindfulness behaviors were less likely to have metabolic syndrome, a high waist circumference, elevated fasting glucose level, or low HDL cholesterol. And a study published in Frontiers in Psychology found that 20 sessions of the mindfulness technique of diaphragmatic breathing helped reduce participants’ salivary cortisol concentration. Such slower breathing practices, often used in yoga and meditation classes, can help decrease fight-or-flight activity while activating the calming components of the parasympathetic nervous system.
But the burden is not placed on each person alone. Khubchandani says policymakers also must take the initiative to effect change at the community, state, and federal levels to help people and families prevent and cope with ACEs. “The key role has to be played by social, cultural, economic, and political factors that can help ensure that children have the optimum climate for growth and development,” he says.