This article was originally posted on the VIM blog, Dr. Joseph’s site covering metabolic health and fitness. It is reposted here with permission.
My patients often enthusiastically share that they are consuming plenty of fruits and vegetables. “I am eating apples, bananas, and watermelon every day now,” a patient recently shared. “But I still can’t seem to shed this weight,” he added, perplexed.
“Fruits and vegetables are not the same. Lumping them together is a crude public health messaging strategy.”
The adage “eat your fruits and vegetables” rolls off the tongue reflexively. In our lexicon, fruits and vegetables go together like knife and fork, cream and sugar, salt and pepper. Perhaps our parents pleaded with us to eat our fruits and vegetables at the dinner table. In elementary school, we learned the health benefits of fruits and vegetables. This was reinforced by public health campaigns, starting back in the early 1990s with the “5 A Day For Better Health” Program, which then morphed into the Fruits & Veggies—More Matter initiative. The USDA’s 2020-2025 dietary guidelines suggest an adult consuming 2,000 calories per day should be eating two and a half cups of vegetables and two cups of fruit per day. The MyPlate icon represents this visually with half of a plate filled with fruits and veggies.
This advice is well-intentioned given that U.S. adults average a meager one serving of fruit and one and a half servings of vegetables per day. Fruits and veggies are packed with health-promoting and disease-fighting nutrients. A large meta-analysis of 26 studies, which involved a total of more than 1.8 million participants reports that eating an average of five servings of fruit and veggies per day is associated with a 13% lower risk of death than eating only two servings per day. Higher intake of fruits and vegetables confers health benefits, reduces the risk of disease, and probably increases longevity. “Eat more fruits and vegetables” is perhaps the safest maxim in a dietary landscape that has been confounded by controversy, fractured into factions, and littered with landmines.
But fruits and vegetables are not the same. Lumping them together is a crude public health messaging strategy.
Fruits and vegetables are botanically distinct. A fruit develops from the flower of a plant, while the other parts of the plant are categorized as vegetables. Fruit (including tomatoes, avocados, and cucumbers) contains seeds, while vegetables can consist of roots, stems, and leaves.
Anyone who has ever eaten a chunk of pineapple and a head of broccoli knows that fruits and vegetables taste different. Fruits generally have a sweet or tart flavor and can be used in desserts, snacks, or juices. Vegetables have a more mild or savory taste and are usually eaten as part of a side dish or main course.
Sure, fruits and vegetables are both high in vitamins, minerals, and antioxidants and low in sodium and fat. But vegetables are generally more nutrient-dense in key vitamins and minerals like potassium, vitamin C, and antioxidants. Given their sweet taste, fruits tend to have a higher amount of sugar and calories compared to most varieties of vegetables. One cup of that pineapple has 82 calories and 16 grams of sugar compared to 31 calories and 2 grams of sugar per cup of broccoli.
Due to differences in nutritional biochemistry, fruits and vegetables are metabolized differently. Compared to most vegetables, particularly the leafy green varieties, fruit is full of fructose, a simple sugar that is metabolized almost exclusively by the liver, where it promotes the synthesis and storage of fat. By contrast, its related but distinct counterpart glucose raises our blood sugar levels and, aided by insulin, enters every cell in our body to provide energy.
In our evolutionary history, sweet was a rare taste found in a beehive or a seasonal fruit. The sweetest fruits in nature were notoriously difficult for our ancestors to access. Tropical fruits like mangos, papaya, pineapples, and bananas grow high on trees. Usually, they are encased in tough skins or shells that are difficult to breach. The physical labor of procuring and opening the fruit was once the only way to the nectarous reward inside. Nowadays, massive servings of perfectly cut, selectively bred, fresh fruit line the shelves of your local supermarket.

Tropical fruits typically had a tough outer layer and grew high in trees, which limited how much of them (and their high fructose) we could eat.
Scientists posit that our ability to convert the fructose in fruit to fat conferred an evolutionary advantage—a backup energy source—to survive periods of famine. It is increasingly clear, however, that our bodies are not adapted to handle the excessive loads of sugar and fructose in particular. Although we often distinguish these “natural” sugars in fruit from added sugars in processed food, our bodies don’t distinguish between a molecule of fructose, glucose, sucrose, or whatever other sugar molecule you consume.
Although it is by no means the driving force, excessive fruit consumption does not help to curb the pandemic of obesity and metabolic disease. Of course, fruit is a healthier alternative to desserts and junk foods, but noshing on fruit all day makes it hard to lose weight. After all, a banana comes with the same amount of carbohydrates as two slices of bread. And fruit, when eaten alone, causes a blood sugar roller coaster that triggers cravings for foods that will quickly raise the blood sugar again—something sweet, like more fruit. Excessive fructose may actually increase our appetite by increasing ghrelin, the hunger-stimulating hormone, and reducing leptin, the hormone that signals satiety. And fructose preferentially activates the reward centers in the brain, which underlie those relentless sweet cravings.
High fructose loads cause cellular inflammation and stimulate the storage of energy in the form of fat. The buildup of fat, or steatosis, in the liver can lead to nonalcoholic steatohepatitis which is often the first manifestation of metabolic dysregulation. So-called metabolic syndrome, which starts with insulin resistance, is the root cause of the major killers in modern society—cardiovascular disease, many cancers, and Alzheimer’s disease. This dysfunction in our metabolism generally traces back to the foods we eat.
To be clear, the total nutritional package in which the sugar resides matters most. Refined and added fructose, particularly in the form of high fructose corn syrup, increases the risk of diabetes and heart disease. Drinking sugar—in the form of sugar-sweetened beverages and fruit juice—is the biggest health offender because the concentration and speed of fructose absorption likely drive insulin resistance and dyslipidemia. Whole fruit is definitely the least harmful offender. The fiber in a whole apple will regulate digestion, increase feelings of satiety, and slow the breakdown and absorption of sugar into the bloodstream. And given the high water and fiber content which discourages overconsumption of whole fruit, it makes sense that some studies find an association between fruit consumption and weight loss.
But proper nutrition necessitates nuance, not soundbites and slogans. Most of the nutrition studies upon which we base our dietary recommendations are observational, based on epidemiological data which by definition cannot prove that eating more fruits and vegetables reduces the risk of death. And most of these studies lump fruit and vegetable consumption together, despite these important differences. That aforementioned whole apple has been selectively bred to be much larger, sweeter, and shinier than its wild ancestors. Overdoing it on the fruit can substantially contribute to the 150 pounds of sugar that Americans consume on average each year.
Given the excessive sugar in our current food environment, I familiarize my patients with the glycemic index, a numerical metric that describes how quickly foods break down into simple sugars in your body. Foods that are high in complex carbohydrates like whole grains and high in fiber have a low glycemic index. By contrast, foods that are high in simple carbohydrates (i.e. sugar) and low in fiber have a high glycemic index. Berries and citrus fruits which are more tart than sweet have less sugar content and a lower glycemic index as compared to tropical fruits like bananas, mangoes, and pineapple. Opting for low glycemic foods keeps our energy levels steady and minimizes big boluses of fructose, craving-inducing fluctuations in blood sugar, and excessive insulin production.
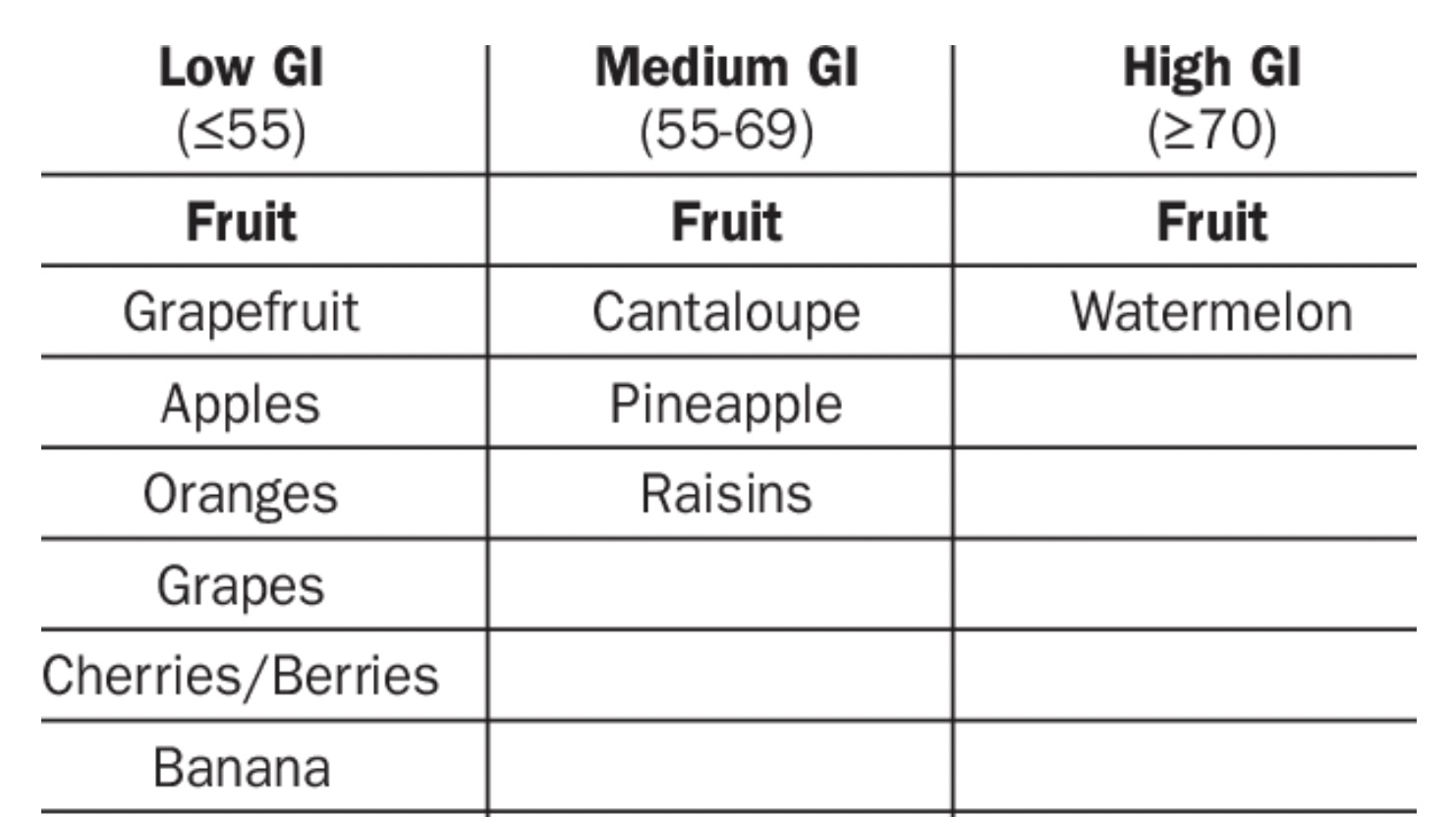
Glycemic index of common fruit. (Image source.)
In my dietary pattern, fruits are an additive to vegetables. Not a replacement for them. I eat fruits as a dessert, and definitely along with some protein and healthy fats to blunt the effect of the sugar load. If we insist on lumping fruits and vegetables together, a more apt public health message would be “Eat your low glycemic fruits and green leafy vegetables.” Sure, a bit more complex. But so is your biology.








